8 Practical Tips for Accurate Home Blood Pressure Monitor Use
Home blood pressure checks give you a clearer picture than a single clinic reading. They help you and your doctor see trends and decide on treatment. Many families in India watch their elders' readings after chai or before the evening walk. A reliable routine stops confusion when readings jump or fall unexpectedly. This guide focuses on easy, research-backed steps you can follow at home, whether you use a basic automatic monitor or a model that syncs with a phone. Follow these tips and you’ll avoid common mistakes that change readings by large amounts. For example, the cuff size and how you sit can shift measurements by 10–40 mmHg, so small fixes matter. We'll cover selecting a validated monitor, getting the cuff fit right, preparing before measurement, posture, timing, multiple-reading methods, logging trends, and device care. Read these tips one at a time and try them out over a week. You’ll soon find a simple routine that fits your day — perhaps after your morning tiffin or before you call dadi. If you have new symptoms or unexpected high averages, contact your doctor. Consistent home monitoring helps you and your clinician make better decisions together.
1. Pick a clinically validated upper-arm monitor
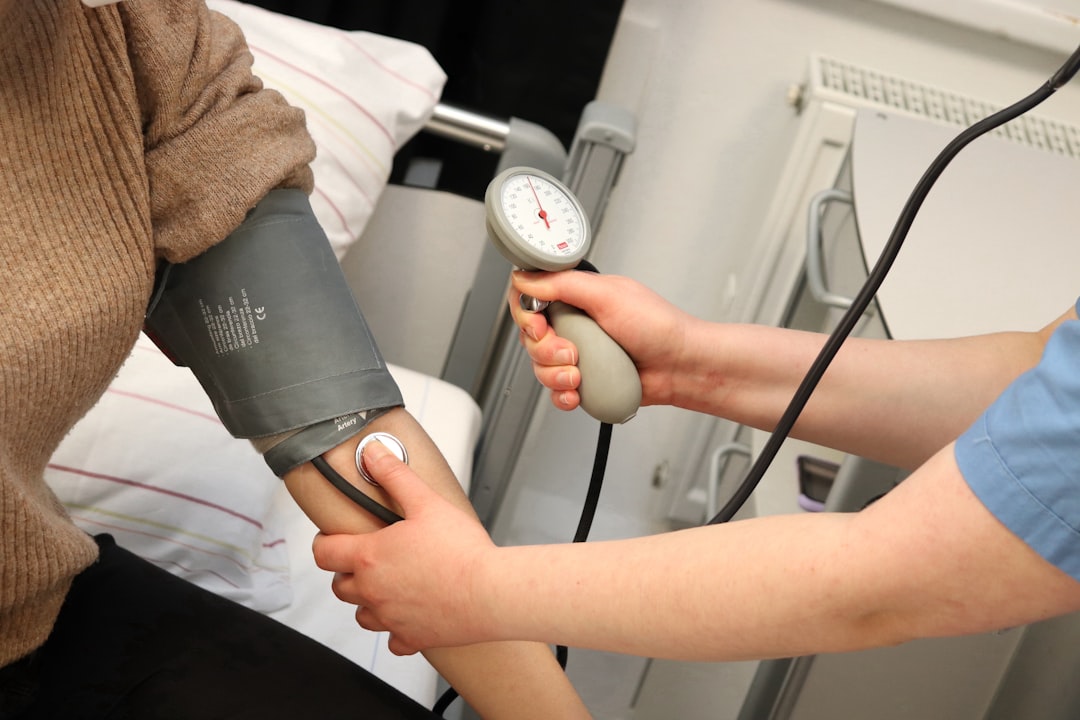
Choose an upper-arm automatic monitor over wrist or finger devices for everyday checks. Major medical groups recommend validated upper-arm models because they give more dependable readings. Look for phrases like "clinically validated" or endorsements from the American Heart Association or equivalent testing groups on the box or product page. Consumer testing sources also compare models for accuracy and reliability. If you want tech features, pick a model that syncs readings to your phone or to cloud storage, but don’t trade accuracy for fancy apps. When shopping in local stores or online marketplaces in India, check reviews and seek retailers who can confirm cuff sizes available for that model. Avoid one-off wrist monitors for routine measurement — they’re more sensitive to hand position and may mislead you. Buy from a brand with a visible service or warranty policy so you can get repairs or calibration help later. Taking time to choose a validated upper-arm monitor reduces false alarms and improves the usefulness of every reading you record.
2. Check cuff size and fit properly

The cuff must match your upper-arm size. Measure around the widest part of the bare upper arm with a tape. The correct cuff typically covers about 80% of the arm circumference and sits roughly 2 cm above the elbow crease. Using a cuff that’s too small can raise readings by a large margin; research reports errors up to 10–40 mmHg from a poor fit. Many monitors come with "medium" cuffs that suit average adults, but larger or smaller arms need alternate sizes. If you care for elderly family members, measure their arms too — age and body changes affect cuff choice. When placing the cuff, make sure it’s snug but not tight, and that the tubing runs down the arm toward the wrist. Always put the cuff on bare skin, not over fabric, because even thin clothing can alter results. If a manufacturer's replacement cuff is available locally, keep one as a spare so you can avoid improvising with an ill-fitting band.
3. Prepare before measuring

Create a short ritual before each reading. Sit quietly for 5–10 minutes to let your pulse and blood pressure settle. Avoid caffeine, tobacco, heavy meals, and vigorous exercise for at least 30 minutes beforehand, since these can raise numbers by several points. Use the restroom if needed because a full bladder can slightly elevate readings. Take off tight-sleeved clothing so the cuff sits on bare skin. Breathe slowly and relax your shoulders; try not to talk during the measurement. If you’ve just come home from work or walked upstairs, give yourself time to rest. A consistent pre-measurement routine reduces random variation and gives readings that reflect your usual level rather than short-term spikes. Apps and simple timers can remind you to wait the right amount of time. Over a week, you’ll see how small preparation changes help create steady, comparable values for you and your clinician to discuss.
4. Sit correctly: posture and arm position

Posture matters. Sit with your back supported and both feet flat on the floor — avoid crossing your legs. Rest your arm on a table or pillow so the cuff sits at heart level; if the arm is too low or too high, readings will be inaccurate. Keep the arm relaxed and still while the cuff inflates and deflates. Use a chair with a firm back rather than a soft sofa, and check that your upper arm rests comfortably on a surface at mid-chest height. If you need a small cushion to raise the arm, that’s fine. Try to stay silent and avoid moving or speaking during measurement because motion can push the numbers higher. A short household trick: place a rolled towel on the table to support the elbow and keep the cuff aligned with the heart. Practicing the same posture each time reduces variability so readings are easier to compare across days.
5. Time it right: set a consistent schedule
Measure at the same times each day for meaningful trends. A common routine is one reading in the morning before medications or breakfast and another in the evening. Blood pressure naturally shifts through the day, sometimes by 10–20 mmHg, so consistency matters more than isolated values. If your doctor asked for pre- and post-medication readings, follow that plan exactly for a few weeks so they can compare impact. Avoid taking measurements just after a stressful phone call or immediately following exercise. On weekends or travel days, keep the timing similar to your home schedule where possible. Mark readings with the time and whether they were before or after a dose. Over two weeks you’ll build a pattern that tells a clearer story than a single measurement, and it makes discussions with your clinician more productive.
6. Take multiple readings and average them
Take two to three consecutive readings, one to two minutes apart, then average the last two. The first reading can be higher as your body settles into the measurement, so averaging gives a steadier estimate. If a single reading is an obvious outlier compared with your usual pattern, take another and record all values. Some monitors automatically display an average if you program multiple readings; otherwise, calculate the mean manually. Keep a note of the arm used, since readings can differ slightly between arms. When you report numbers to a doctor, use the averaged value for that session rather than a single spike. Many health professionals suggest discarding the first measurement when it's much higher and using the next two. This routine reduces random error and gives a reading your clinician can trust for treatment decisions.
7. Log, track, and share trends with your doctor

Record the date, time, arm used, and each reading plus any symptoms like dizziness or headache. A simple notebook works well and can sit next to the monitor in your kitchen or bedroom. If you prefer digital tools, choose a trusted app that stores dates and times and can export or show trends. Many modern monitors can sync readings automatically to phones, but double-check data accuracy after syncing. Trends over weeks are more important than isolated highs. When visiting the clinic, bring printouts or screenshots so the doctor sees patterns and not just single numbers. If family members share monitoring duties, keep the log accessible so everyone adds entries consistently. Good records help avoid unnecessary medication changes based on one-off readings and make it easier to spot real trends that need clinical attention.
8. Maintain and calibrate your device regularly

Treat your monitor like any medical tool. Replace batteries before readings start to fade, keep the cuff clean and free of cracks, and store the monitor in a dry spot. Many manufacturers advise an annual calibration or check to ensure ongoing accuracy; follow their guidance and local service options. If your monitor falls or acts strangely, stop using it until verified. Some newer models include self-checks that flag errors, while older units may need professional testing at a clinic or vendor. Avoid using damaged cuffs or taped repairs — these can change readings. Keep the original manual and warranty information so you know the recommended maintenance schedule. Proper care extends the device’s life and prevents misleading measurements that can cause worry or incorrect treatment changes.
Wrap-up: small habits, clearer readings
Reliable home blood pressure monitoring comes from a few steady habits: choose a validated upper-arm monitor, use the correct cuff, prepare and sit properly, measure at consistent times, take multiple readings, log results, and keep the device in good condition. These steps keep readings honest and useful when you and your clinician make decisions together. In Indian homes, where elders and younger family members share health duties, a clear routine makes monitoring simple and less stressful. If you notice sustained high averages or troubling symptoms, reach out to your healthcare provider with your logged data. Small, regular actions give better insight than occasional panic checks, and they help you manage blood pressure with more confidence. Keep the monitor handy, agree on a time that fits your household rhythm, and let consistent tracking guide better conversations with your doctor.
