11 Natural Methods for Period Pain Relief That Actually Help
Period cramps can make ordinary days feel heavy. Many people reach first for an over-the-counter pill, and that works well for some. Others want natural options that blend quick relief with longer-term care. This guide lists 11 evidence-backed methods you can try at home or with a practitioner, mixing simple daily habits and time-tested remedies. Each method includes what the research says, practical steps, and safety notes so you can make smart choices. We kept the advice practical and culturally grounded. If your dadi suggested warm haldi milk for pain, you’ll see how turmeric fits a modern anti-inflammatory approach. If yoga helps you feel better, there are pose options and stretches to try. Sources include reputable medical sites and peer-reviewed summaries so the suggestions are evidence-forward and North America–relevant. If your cramps are severe, sudden, or getting worse, see a clinician—these tips are for typical menstrual cramps, not emergency symptoms. Use this list to mix short-term relief with long-term strategies, and track what helps you best.
1. Heat therapy: targeted warmth for fast relief

Using heat on your lower belly or back is one of the simplest and most reliable ways to ease cramps. Studies and clinical reviews note that topical heat can match or even outperform some over-the-counter pain relievers for menstrual pain by increasing local blood flow and relaxing uterine muscles (Health.com). Try a heating pad, hot water bottle, or a warm bath for 15–20 minutes at a comfortable warmth. Many sources suggest keeping the temperature around 40°C (104°F) to feel soothing without overheating. Apply heat as soon as cramps start, and repeat several times a day if it helps. Heat is safe for most people. Don’t use a hot surface directly on numb skin or over broken skin. If you have diabetes, neuropathy, or reduced sensation, test temperature carefully and talk to your provider before using long sessions. Combining heat with a gentle belly massage or a warm bath can add relaxation. Image suggestion: heating pad on abdomen. Alt text: "Heating pad on lower abdomen for cramp relief."
2. Gentle exercise and yoga: move to ease cramping

Moving your body helps. Regular aerobic exercise and targeted yoga both reduce menstrual pain over time by boosting endorphins and improving circulation. Clinical guidance often recommends about 45–60 minutes of activity most days for overall benefits, and even low-intensity sessions can ease symptoms during your period (Health.com, NHS). On heavy-cramp days, keep it gentle. Try walking, a short yoga flow, or restorative poses such as child's pose, supported bridge, and reclining twist. These poses gently stretch the low back and pelvis and can relieve tension. Aim for several short sessions if a single long workout feels rough. Even 10–20 minutes of movement can help your mood and pain perception. If you’re new to exercise, start slowly and increase intensity gradually. Avoid high-impact workouts if they make bleeding heavier or pain worse. For tailored sequences, consider a certified yoga instructor familiar with menstrual modifications. Image suggestion: child's pose yoga. Alt text: "Person in child's pose on yoga mat at home."
3. Acupressure and acupuncture: pressure points you can try

Acupuncture and acupressure are traditional techniques that many studies show can reduce primary menstrual pain. Acupuncture involves thin needles placed by trained practitioners, while acupressure uses firm pressure on points such as SP6 (located above the inner ankle) to ease cramping. Reviews suggest both approaches are generally safe and may lower pain scores in people with dysmenorrhea (Health.com, PubMed reviews). For self-care, use firm but gentle pressure for 2–3 minutes per point, several times a day. Combine acupressure with warmth or a light abdominal massage for added benefit. If you opt for professional acupuncture, look for licensed practitioners and tell them about any health conditions or blood-thinning medications. Be cautious if you have a bleeding disorder or use anticoagulants—needle-based therapies may not be appropriate. Also avoid self-acupressure on spots that cause sharp pain or on areas with skin problems. Image suggestion: acupuncture session. Alt text: "Licensed acupuncture session focused on lower body."
4. Aromatherapy and essential-oil massage for gentle relief

A short abdominal massage with diluted essential oils can ease cramps by combining soothing scent with gentle pressure. Oils such as lavender, fennel, peppermint, or rose have small clinical studies showing benefit when massaged into the lower tummy for 10–15 minutes (Health.com). Always dilute essential oils in a carrier oil like coconut or almond oil—usually a 1–2% dilution (1–2 drops of essential oil per teaspoon of carrier). Massage with light circular motions for several minutes, repeating as needed. Aromatherapy also supports relaxation, which can reduce pain perception. Avoid certain oils during pregnancy and patch-test new oils on your inner arm for reactions before abdominal use. If you have sensitive skin or eczema, consult a dermatologist. Using oils alongside heat or a warm compress often enhances the soothing effect. Image suggestion: lavender essential oil. Alt text: "Small bottle of lavender essential oil with fresh lavender sprigs."
5. Ginger: a time-tested anti-inflammatory tea or supplement

Ginger is one of the most studied herbs for menstrual pain. Small trials and meta-analyses suggest that ginger can reduce cramp severity, sometimes to a level comparable with standard NSAIDs, by decreasing prostaglandin activity and inflammation (Health.com, PubMed summaries). Common approaches include fresh ginger tea, ginger powder in food, or standardized supplements. Typical dosing in trials ranges from 500 mg to 1,000 mg of powdered ginger daily during the first 2–3 days of bleeding. To make tea, steep fresh slices or grated ginger in hot water for 10 minutes and sip warm. Ginger also pairs well with haldi (turmeric) and honey for a comforting drink. Ginger can thin the blood slightly and may interact with blood-thinning medications, so check with your healthcare provider if you take anticoagulants. Also watch for heartburn in people prone to reflux. Image suggestion: ginger tea. Alt text: "Cup of fresh ginger tea with sliced ginger on a saucer."
6. Cinnamon: a simple spice with clinical backing

Cinnamon has anti-spasmodic and anti-inflammatory properties and shows benefit in some trials for menstrual pain. In randomized studies, supplementing with about 1,000 mg of cinnamon in the early days of the period reduced pain intensity compared with placebo (Health.com). You can add cinnamon to warming drinks like chai or haldi milk, stir it into porridge, or take it as a standardized capsule if you prefer a measured dose. When using whole cinnamon, remember there are two common types: Ceylon (true) cinnamon and cassia. Cassia contains more coumarin, which at high amounts can affect the liver, so avoid very large regular intakes of cassia-based supplements. If you have diabetes or use medications that affect blood sugar, monitor levels closely when adding large amounts of cinnamon and consult your clinician about safe doses. Image suggestion: ground cinnamon. Alt text: "Spoonful of ground cinnamon with cinnamon sticks nearby."
7. Chamomile tea: cozy, calming, and muscle-relaxing

Chamomile has mild muscle-relaxing and anti-inflammatory constituents and has shown benefit in small trials for easing menstrual cramps and improving sleep. A warm cup before bed can help relax pelvic muscles and lower stress, both of which reduce pain perception (Health.com). Brew chamomile tea for 5–10 minutes and sip warm; some people combine it with honey or a pinch of cinnamon. The calming effect also helps if cramps interfere with sleep. For a stronger effect, try a few cups spread across the day, particularly on the first 48–72 hours. Chamomile can interact with certain sedatives and may trigger allergic reactions in people who are sensitive to ragweed or related plants. Avoid heavy use with potent sedative medications; discuss combinations with your clinician. Image suggestion: chamomile tea. Alt text: "Cup of chamomile tea with chamomile flowers on a table."
8. Omega-3 fatty acids: reduce inflammation from the inside

Omega-3 fatty acids (EPA and DHA) cut inflammation and can lower menstrual pain and the need for painkillers. A review of trials shows benefit, with effective supplement dosing commonly ranging from about 300 mg up to 1,800 mg daily taken for several weeks to months for best results (Dr. Ruscio, PubMed meta-analyses). Food sources such as salmon, mackerel, sardines, and flaxseed oil also help. If you choose supplements, look for third-party tested fish oil or algae-based omega-3s (for a vegetarian option) and follow label dosing or clinician guidance. Start a few weeks before expected symptoms if you can, since dietary changes often take time to shift inflammation levels. Note that high-dose omega-3s can increase bleeding risk when combined with anticoagulant drugs, so discuss supplements with your provider if you are on blood thinners. Image suggestion: salmon fillet. Alt text: "Cooked salmon fillet with lemon wedge and herbs."
9. Magnesium and calcium: minerals that help muscle function
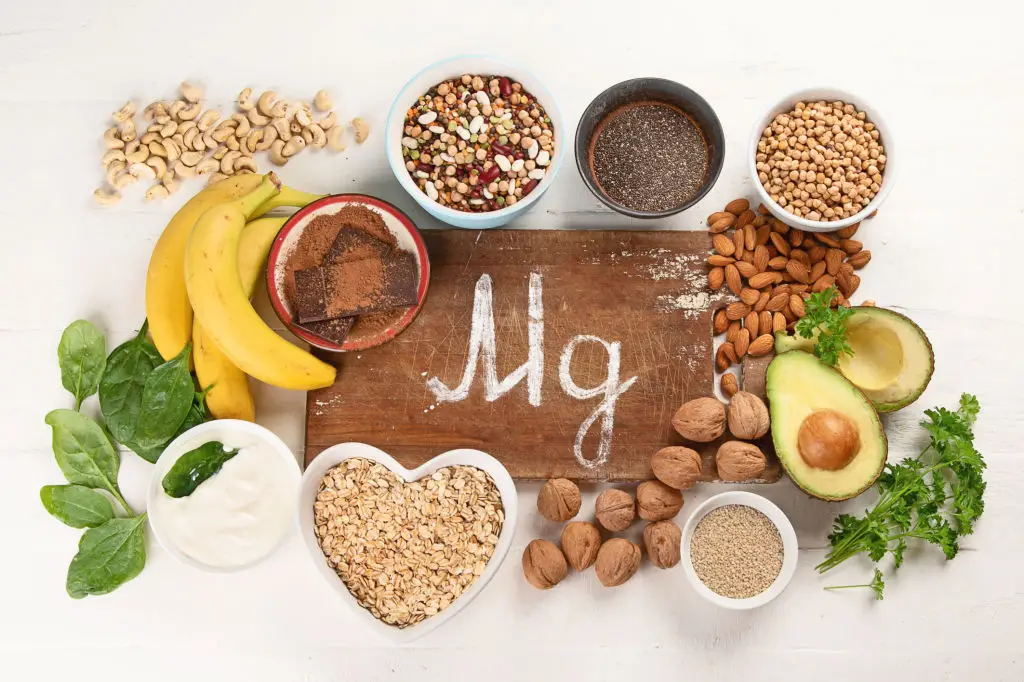
Magnesium helps muscles relax and may reduce cramps when taken regularly, and calcium supports muscle and nerve function. Studies indicate that people with PMS often have lower magnesium and calcium; supplementing or eating mineral-rich foods can improve symptoms for some (Dr. Ruscio, Mayo Clinic guidance). Magnesium-rich foods include pumpkin seeds, chia, almonds, and leafy greens. Calcium is abundant in yogurt, milk, paneer, and small fish with bones. If using supplements, typical magnesium doses in studies range from 200–400 mg daily, but talk to your clinician first to choose the right form and dose. People with kidney disease should avoid unsupervised high-dose magnesium. Also be mindful of interactions with certain medications, including some antibiotics and diuretics. Favor food sources when possible and use supplements under medical advice. Image suggestion: magnesium rich foods. Alt text: "Bowl of mixed seeds and nuts high in magnesium."
10. Anti-inflammatory diet and hydration: long-term cycle care

What you eat across the month matters. Diets higher in whole foods and lower in refined sugar and processed fats tend to reduce inflammation and may lead to milder cramps over time. Focus on vegetables, legumes, whole grains, fatty fish, nuts, and anti-inflammatory spices like turmeric (haldi), which pairs well with black pepper for better absorption (PubMed reviews, NHS nutrition guidance). Try simple swaps: swap sugary snacks for fruit, add a turmeric-spiced dal or a turmeric latte (haldi doodh) as a bedtime ritual, and include regular servings of fatty fish or flaxseeds. Hydration helps too—aim for steady fluids and moderate sodium to avoid bloating-related discomfort. If you have specific dietary needs or conditions like IBS or food intolerances, tailor the plan with a registered dietitian. Dramatic changes overnight aren’t needed; gradual shifts often stick better and give clearer feedback about what helps your cramps. Image suggestion: healthy anti-inflammatory meal. Alt text: "Colorful plate of anti-inflammatory foods with vegetables and grains."
11. Stress reduction, sleep, and soothing routines

Stress changes how your brain interprets pain, so calming routines can lower menstrual discomfort. Practices such as diaphragmatic breathing, short guided meditations, progressive muscle relaxation, and prioritizing good sleep often reduce the intensity of cramps. Clinical sources link better sleep and lower stress to reduced pain perception (Mayo Clinic). Build a simple nightly ritual: a warm bath, gentle stretching, a cup of haldi doodh (warm milk with turmeric and black pepper) or chamomile tea, and 10 minutes of breathing exercises. These steps help the nervous system downshift and can make cramps feel less severe. If anxiety or poor sleep are chronic, consider talking to a mental health provider. If pain is tied to heavy anxiety, professional treatment can be an important part of the solution. Track which relaxation habits make a measurable difference so you can repeat what helps each month. Image suggestion: meditation practice. Alt text: "Person practicing seated meditation indoors with soft lighting."
Wrapping up: mix and match the methods that work for you

Finding reliable period pain relief often means combining quick fixes and longer-term habits. Heat and a short abdominal massage can ease acute cramps. Gentle movement, yoga, and acupressure add non-drug relief. Herbs like ginger and cinnamon, chamomile, minerals such as magnesium, and omega-3s all have evidence for benefit when used thoughtfully and safely. Diet and stress reduction support lower pain across cycles, and a culture-rooted touch—like haldi doodh or a family balm—can add comfort while fitting into modern care. Always check safety: some herbs and supplements interact with medications or are not recommended during pregnancy. If cramps are severe, get medical evaluation to rule out conditions like endometriosis or fibroids. Try one or two methods at a time, track results, and consult your healthcare provider when needed. With gentle experiments and evidence-based choices, many people reduce both the intensity and frequency of period pain without relying only on medication.
