11 Preventive Health Screening Tests Doctors Recommend
Preventive health screenings are the simplest way to catch problems early and keep you well. Doctors use these tests to find conditions before they cause symptoms, which often makes treatment easier and outcomes better. This guide covers 11 tests physicians commonly recommend for adults in the U.S. and explains who should get each test, what to expect, how often to do it, and simple preparation steps. The recommendations below draw on major authorities (U.S. Preventive Services Task Force, American Cancer Society, CDC, and major medical centers). They aim to be practical and user-friendly so you can talk confidently with your clinician and plan appointments around daily life. For example, scheduling a fasting blood draw early before the day’s tiffin or setting a weekday mammogram after work can help you follow through. Screening choices can depend on age, sex, personal and family health history, and lifestyle. Some tests are one-time checks while others are ongoing. A few require a shared decision with your doctor because benefits and risks vary by person. If cost or insurance is a worry, ask your primary care clinic or insurer about coverage — many preventive tests are covered under U.S. plans. Keep this article as a checklist to bring to your next visit. Start with the basics like blood pressure and cholesterol, and use questions in each section to guide a brief conversation with your clinician.
1. Mammography (breast cancer screening)
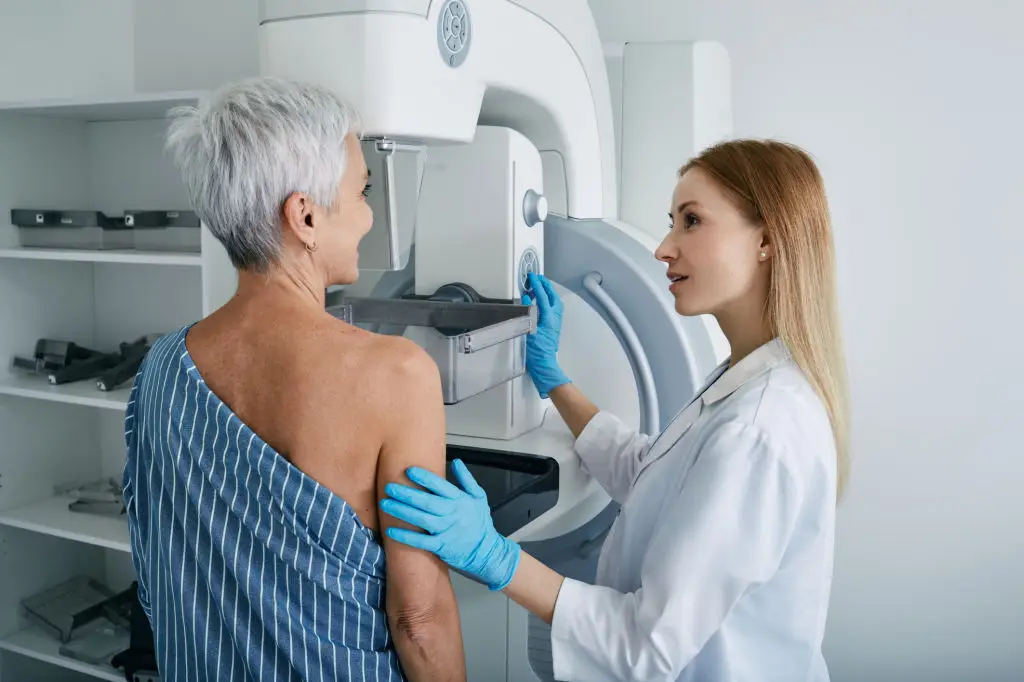
Mammography is an X-ray exam that can detect breast changes before you or your doctor can feel them. Many organizations recommend women begin discussing screening around age 40, with options to start routine mammograms at 40–45 and continue annually or every two years based on personal risk and clinician guidance (American Cancer Society; USPSTF). What to expect: you’ll step into an imaging room, a technologist will position the breast on a platform, and the machine briefly compresses the tissue for two views per breast. The compression can feel firm but is over in seconds. Preparation tips: avoid lotion, deodorant, or powder on the day of the test because these products can show up on the image and may require retakes. Wear a two-piece outfit for convenience and bring prior mammogram images if you’ve had them elsewhere. If you have a strong family history of breast cancer, genetic factors, or dense breasts, ask about supplemental screening (ultrasound or MRI) and earlier or more frequent imaging. After the exam, most clinics release results within days. If your report calls for additional imaging, don’t panic — many follow-ups are routine (American Cancer Society).
2. Colorectal screening (colonoscopy / FIT)
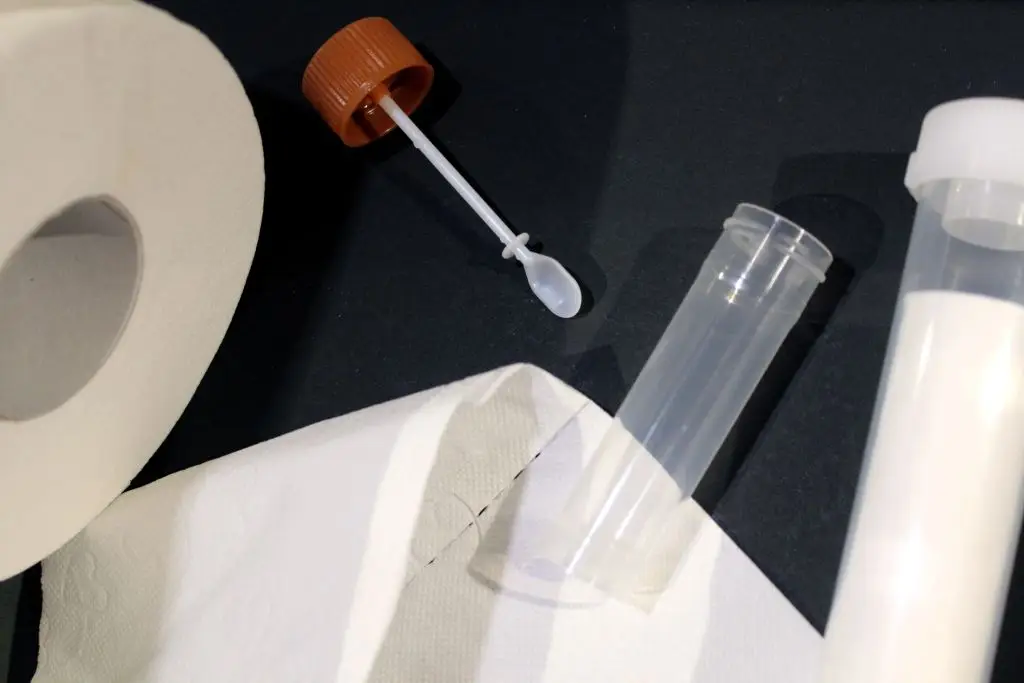
Colorectal screening looks for polyps or early cancers in the colon and rectum. Current guidance recommends average-risk adults begin screening at age 45; options include colonoscopy every 10 years or annual at-home fecal immunochemical testing (FIT) depending on preference and access (USPSTF; American Cancer Society). What to expect for colonoscopy: you’ll follow a clear-liquid diet and take a bowel-prep laxative the day before to empty your colon. On the day, you receive sedation and a physician uses a flexible scope to examine the colon lining; the procedure often takes 20 to 60 minutes. FIT involves a simple stool sample sent to a lab with no prep. Preparation tips: follow bowel prep instructions precisely for a quality exam, arrange a ride home after colonoscopy, and ask your clinic about antibiotics only if you have certain heart or valve conditions. If polyps are found, they can often be removed during colonoscopy, which prevents many cancers. If you live a busy life, FIT kits can be done around home routines and are an effective screening choice when done yearly and followed by colonoscopy if positive.
3. Cervical screening (Pap/HPV)

Cervical screening detects abnormal cells or high-risk HPV types that can lead to cervical cancer. People with a cervix should start screening at age 21 and continue through about age 65, with Pap tests every three years or co-testing with Pap plus HPV every five years depending on guidelines and prior results (USPSTF; American Cancer Society). What to expect: during a brief pelvic exam, a clinician gently collects cells from the cervix with a small brush or spatula; the sample is sent to a lab. Preparation tips: avoid intercourse, douching, or applying vaginal medicines for 48 hours before the test to reduce false results; schedule around work or caregiving duties as needed. If your results show certain abnormal findings or HPV positivity, follow-up may include a repeat test, an HPV typing result, or a colposcopy for closer inspection. HPV vaccination dramatically lowers risk for several cancer-causing strains; discuss vaccination status with your clinician if you’re eligible. Regular screening and vaccination together have greatly reduced cervical cancer incidence where they’re used widely.
4. Blood pressure check

A blood pressure check is a quick, essential screen for high blood pressure — a top risk for heart disease and stroke. Adults should have their blood pressure checked regularly: at least every two years if readings are normal and more often if elevated or if you have other risk factors (American Heart Association; USPSTF). What to expect: a clinician or nurse will have you sit quietly, place a cuff on your upper arm, and take one or more readings; many clinics average multiple measurements. Home monitoring can help track trends; bring your home device to a visit for calibration. Preparation tips: avoid caffeine, smoking, and exercise 30 minutes before measurement; sit with feet flat and arm supported. If your blood pressure is high, your clinician may suggest lifestyle steps like reducing salt and increasing daily activity, or may start medication depending on overall cardiovascular risk. Regular checks are painless and fit easily before or after a tiffin break, or during workplace wellness visits.
5. Cholesterol/lipid panel
A cholesterol or lipid panel measures blood fats that influence heart disease risk, including LDL, HDL, and triglycerides. For healthy adults, testing typically starts in early adulthood and repeats every 4–6 years if results are in a healthy range; people with cardiovascular risk factors or diabetes are tested more often (AHA; USPSTF). What to expect: a nurse will draw blood, often from the arm. Some clinics ask for fasting before the test, while others accept non-fasting samples — check before your appointment. Preparation tips: confirm fasting requirements with your provider, and avoid heavy alcohol or fatty meals the night before to reduce variability. Results are used with your blood pressure, age, smoking status, and other factors to calculate your 10-year cardiovascular risk and guide whether lifestyle changes or medications like statins are recommended. Discuss family history of early heart disease with your clinician, as that may mean earlier testing or treatments.
6. Diabetes screening (A1C / fasting glucose)
Diabetes screening detects elevated blood sugar that can lead to complications if untreated. Screening is recommended for adults starting around age 35 for those at average risk, earlier or more often if you have overweight, family history, high blood pressure, or other risk factors (ADA; USPSTF). What to expect: common tests include an A1C blood test, which shows average blood sugar over a few months, or a fasting glucose test measured after an overnight fast. Preparation tips: for fasting glucose, avoid food and calorie-containing drinks for 8–12 hours before the test; the A1C usually does not require fasting. If results indicate prediabetes, clinicians will often recommend lifestyle changes like modest weight loss, increased daily activity, and dietary shifts that can delay or prevent progression to diabetes. Many clinics offer brief counseling or refer to community programs; consider scheduling tests at times that fit around work or family routines so follow-up is easier.
7. Bone density test (DEXA)
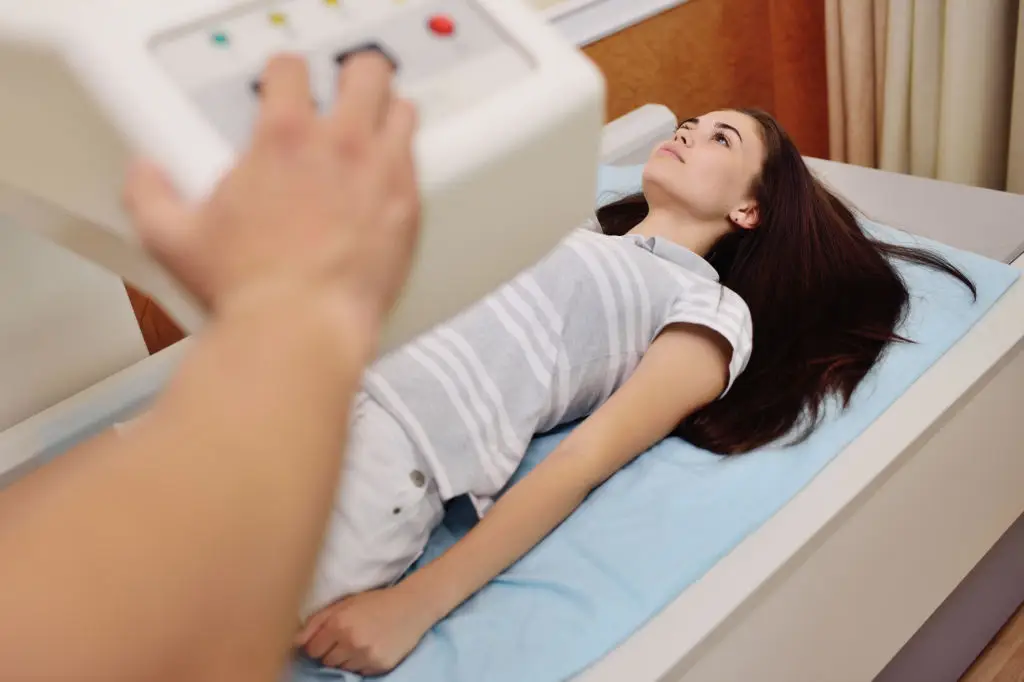
A DEXA scan measures bone mineral density to assess osteoporosis risk, which affects fracture risk as people age. Routine screening is generally recommended for women starting around age 65; younger adults with risk factors (early menopause, chronic steroid use, low body weight, or previous fractures) should discuss earlier testing with their clinician (NOF; USPSTF). What to expect: the DEXA machine scans your hip and spine while you lie on a padded table; the test is painless and takes about 10 to 20 minutes. Preparation tips: wear comfortable clothes without metal and avoid taking calcium supplements on the day of the scan unless instructed otherwise. Results use T-scores to guide management: lifestyle measures like weight-bearing exercise, adequate calcium and vitamin D, and fall-prevention strategies often come first; medications may be recommended for higher fracture risk. If you care for elderly parents or coordinate clinic visits, combining DEXA with other preventive appointments can reduce travel burden.
8. Lung cancer screening (low-dose CT)
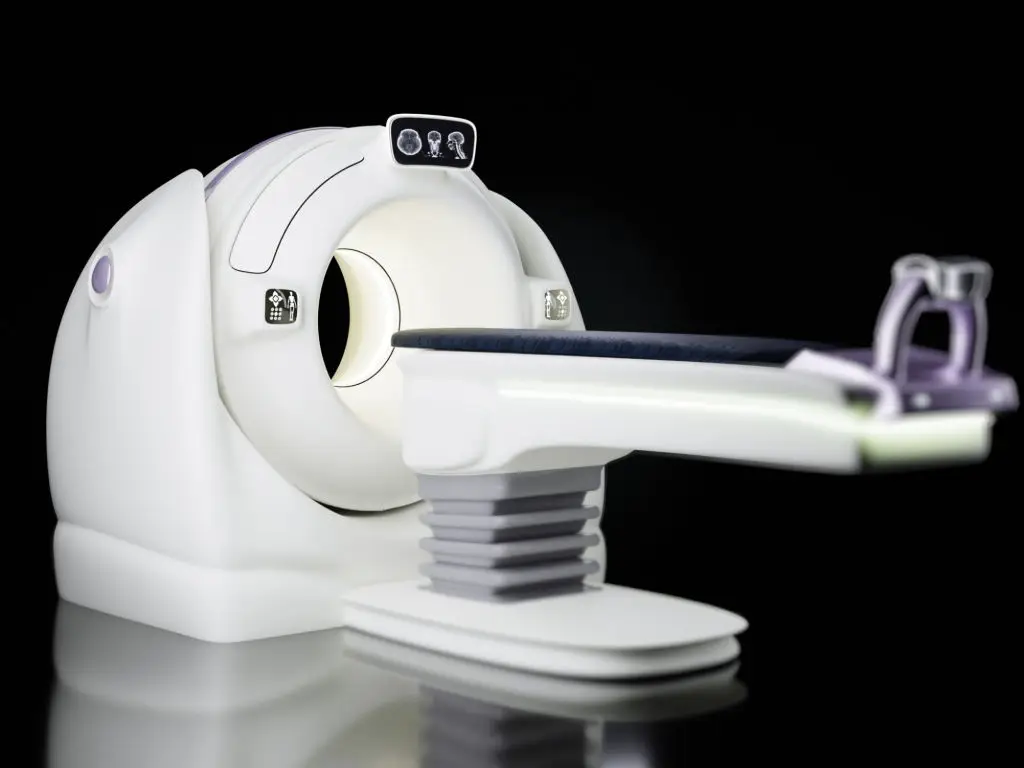
Low-dose CT (LDCT) screening can find early lung cancers in people at higher risk from smoking. Recommended candidates typically include adults aged about 50–80 with a 20-pack-year smoking history who currently smoke or quit within the past 15 years; screening is usually annual while risk remains (USPSTF; American Cancer Society). What to expect: the test is a quick, noninvasive CT scan of the chest without contrast that takes only minutes. Preparation tips: wear loose clothing and leave jewelry at home; no fasting is required. Screening programs emphasize smoking cessation support as a central part of care — quitting lowers future risk even after years of smoking. If a nodule is found, radiologists often use follow-up CTs or other tests to monitor size before more invasive steps. Discuss eligibility and the balance of benefits and harms with your clinician, since false positives and follow-up testing are possible.
9. Prostate screening (PSA / shared decision-making)
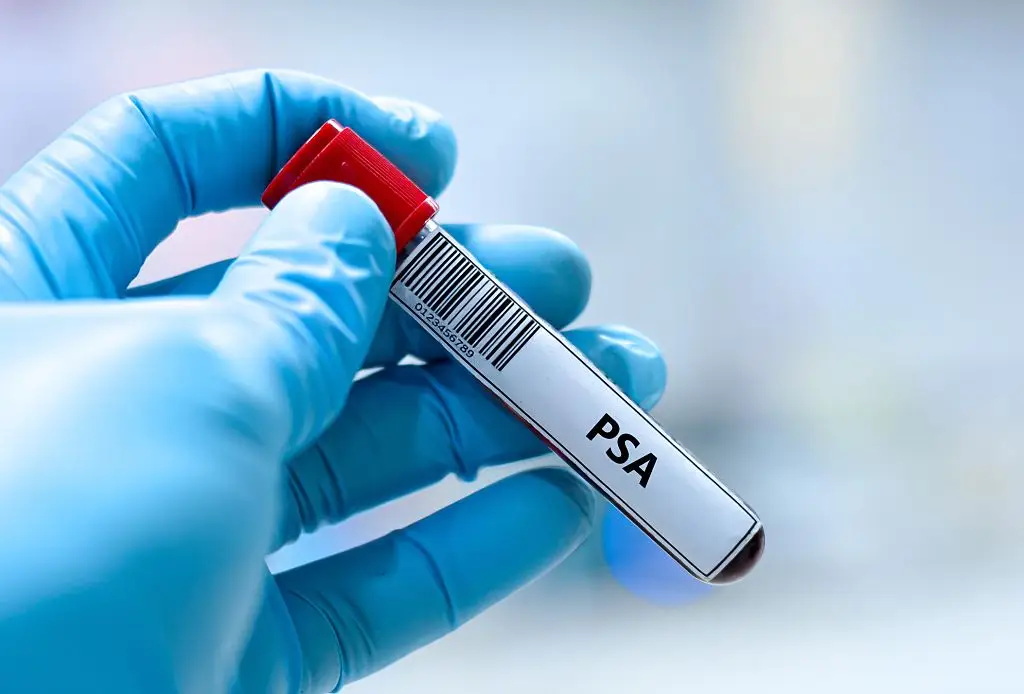
Prostate screening with a PSA blood test can detect prostate changes but carries trade-offs between early detection and overdiagnosis. Major guidance recommends individualized shared decision-making about PSA testing for men roughly 55–69 years old, with some men at higher risk discussing earlier testing (African American men, those with family history) (USPSTF; American Cancer Society). What to expect: a simple blood draw measures prostate-specific antigen levels; elevated PSA often leads to repeat testing and possibly imaging or biopsy. Preparation tips: avoid ejaculation and strenuous prostate stimulation for 48 hours before the test, and tell your clinician about recent urinary procedures that can affect results. Because PSA screening can lead to detection of slow-growing tumors that may never cause harm, many men opt for active surveillance rather than immediate treatment if low-risk cancer is found. Discuss your values, family history, and health priorities with your provider to decide whether PSA testing fits your care plan.
10. Abdominal aortic aneurysm (one-time ultrasound for certain men)
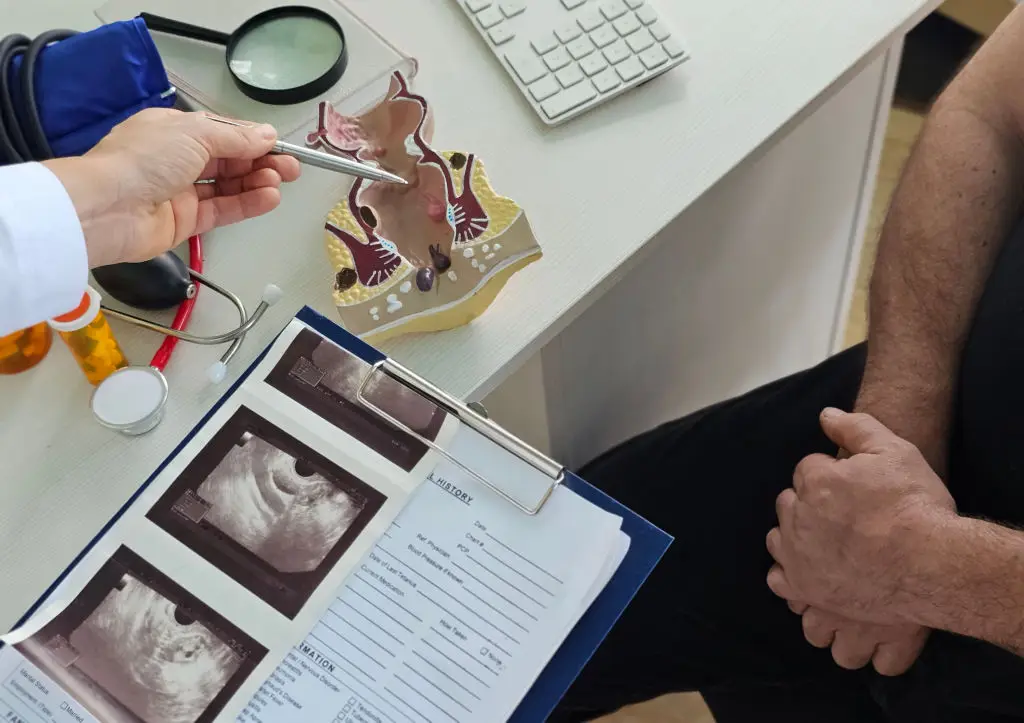
Abdominal aortic aneurysm (AAA) screening uses an ultrasound to look for dangerous enlargement of the main abdominal artery. A one-time ultrasound is usually recommended for men aged 65–75 who have ever smoked; other people with a strong family history or vascular disease should discuss testing with a clinician (USPSTF). What to expect: the ultrasound is noninvasive and brief; you lie on a table while a technician moves a probe over your abdomen. Preparation tips: many centers require no special prep, though some may ask you to avoid heavy meals beforehand. If an aneurysm is detected, vascular specialists may monitor its size with periodic imaging or recommend surgery if it reaches a threshold where rupture risk rises. Early detection through screening has reduced emergency surgeries and deaths in screened populations, especially among former smokers.
11. Hepatitis C screening (one-time or risk-based)
Hepatitis C screening is a blood test that finds a viral infection which can silently damage the liver over years. Recent guidance supports at least one-time testing for most adults and more frequent screening for people with ongoing risk exposures, because highly effective treatments can cure most infections (CDC; USPSTF). What to expect: a simple blood draw is sent to a lab for antibody and confirmatory RNA testing if needed. Preparation tips: no fasting or special prep is required. If you test positive, your clinician will order follow-up tests and, when appropriate, referral to a specialist for antiviral therapy that often clears the virus. Testing is especially important if you have a history of injection drug use, prior blood transfusions before screening of the blood supply, or other exposures. Getting tested removes uncertainty and opens the door to curative treatment for most people.
Wrap-up: Make screenings a simple habit

Regular screening helps catch many serious conditions early when they are easier to treat. Start by keeping a simple checklist with your age and risk factors and use it at annual physicals or telehealth visits. Talk openly with your clinician about tests that need shared decision-making, such as PSA or certain cancer screens, and ask how often your insurance covers each exam. If scheduling is a hurdle, book tests around predictable daily routines — an early morning blood draw before the tiffin or a weekend imaging slot after family duties can make compliance easier. Remember that many screenings are painless or quick: a blood draw, a short scan, or an in-office check can provide valuable peace of mind. Prevention also includes small daily habits like staying active, not smoking, and managing salt and sugar intake. If a test finds something, most results lead to clear next steps rather than immediate alarm. Finally, keep copies of results and any imaging so new clinicians can compare changes over time. Use this list as a conversation starter with your doctor, and tailor the recommendations to your personal health and family history (USPSTF; American Cancer Society; CDC). A short appointment today can avoid bigger problems later, and that’s time well spent on your long-term health.
