13 Science-Backed Metabolic Syndrome Prevention Steps to Reduce Your Risk
Metabolic syndrome quietly raises the odds of heart disease, stroke, and type 2 diabetes. Many people have one or two risk factors already — high waist circumference, high blood pressure, high fasting sugar, high triglycerides, or low HDL cholesterol — and those add up. The good news is that practical habits can push those numbers in a healthier direction. This article lays out 13 simple, research-backed steps you can start using today to lower your risk and protect long-term health. Each step mixes clear science with everyday tips so you can pick the actions that fit your life. For example, a short walk after lunch can blunt a blood-sugar spike, and small swaps in the kitchen can cut daily refined carbs without losing familiar flavors. Sources for key recommendations include clinical reviews and recent studies from trusted outlets such as the Institute for Functional Medicine, peer-reviewed journals, and clinical manuals. Where helpful, we offer culturally grounded options — like using dal and seasonal vegetables or traditional fermented dishes — to make changes easier to keep. Read the list to find practical moves you can try this week, and remember: small consistent changes are what shift long-term risk. If you have health conditions or take medications, check with your healthcare provider before making major changes.
1. Move Daily: Build a realistic exercise plan

Regular physical activity is one of the strongest ways to reduce metabolic syndrome risk. Guidelines recommend at least 150 minutes of moderate activity or 75 minutes of vigorous activity weekly, with added resistance training to preserve muscle and improve insulin sensitivity (IFM, 2025). That sounds formal, but it can be practical and cultural: brisk walks to the market, a game of cricket with friends, or a tiffin-time stair climb can all count. Aim for a mix that raises heart rate and challenges large muscle groups twice a week. Short bouts spread through the day can be easier to keep than long sessions; three 10–15 minute brisk walks add up and help with blood sugar control. Resistance work like bodyweight squats, push-ups, or using water bottles as weights twice weekly will support muscle mass and metabolic health as you age. If mobility or chronic conditions make activity harder, start with seated exercises and build up gradually. Consistency matters more than intensity; small, repeatable movement is better than occasional extremes. If you’re new to exercise, a graded plan and a check-in with your clinician will keep things safe and effective.
2. Walk After Meals: A small habit with measurable benefit
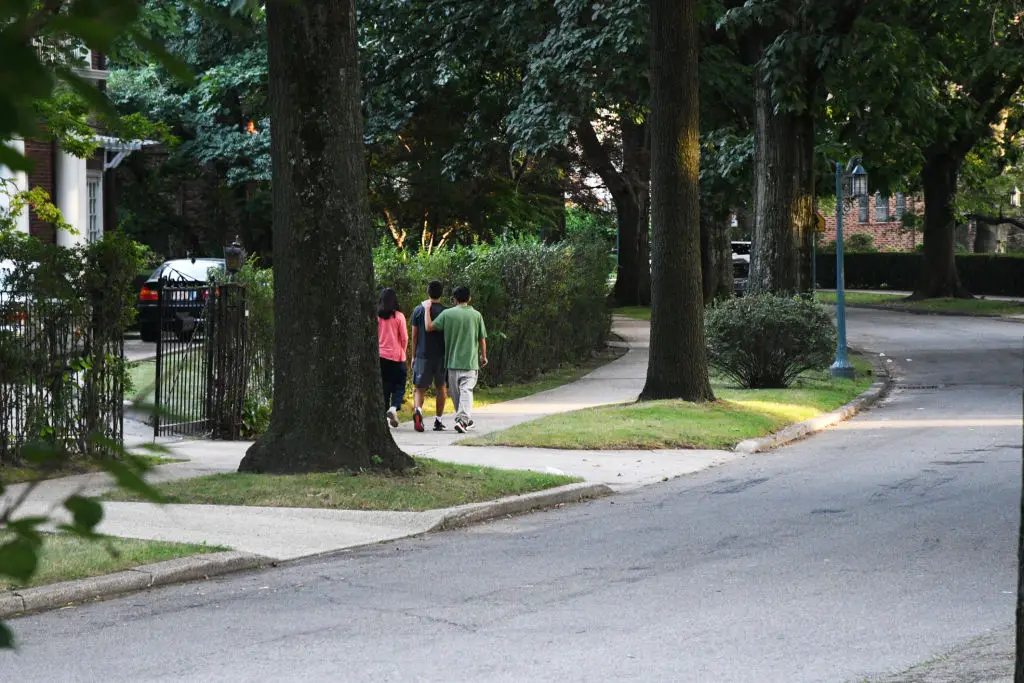
Walking for 10–30 minutes after a meal can significantly reduce post-meal blood sugar spikes. Recent work notes reductions in peak glucose when people take a short walk after eating, sometimes lowering spikes by around 30% for some individuals (News-Medical, 2025). This practice is easy to fit into a tiffin or lunch break: a 10–15 minute stroll after the midday meal at the office, or a gentle walk after dinner with the family. It doesn’t need to be fast; steady movement that engages leg muscles helps skeletal muscle take up glucose and eases the burden on insulin. If neighborhood safety or weather is a concern, marching in place or stepping up and down a single stair at home are valid alternatives. For people with mobility issues, seated leg extensions or ankle circles after meals can offer benefit. Try making it a family habit: a post-meal walk becomes social time, reduces screen time, and supports digestion. Over weeks, this habit can help lower average blood sugar and make other lifestyle changes more effective.
3. Adopt a Mediterranean-style pattern with Indian swaps

A diet rich in vegetables, legumes, whole grains, healthy fats, and lean proteins protects metabolic health. Studies and clinical guidance support Mediterranean-style patterns for improving weight, lipids, and blood sugar control (IFM, 2025). You don’t need to copy a European menu: use familiar ingredients in new combinations. Make dals and sabzis the center of the plate, choose brown rice or millets instead of refined white rice regularly, and add healthy fats like small amounts of cold-pressed mustard or groundnut oil, and nuts for snacks. Swap fried snacks for roasted chana or spiced buttermilk to cut refined carbs and excess calories. Increasing vegetables at each meal and choosing whole pulses or mixed-grain rotis helps with fiber and slow glucose absorption. Aim for more plant-based meals across the week, with fish or lean poultry a few times if preferred. Portion awareness matters: a balanced plate halves vegetables, quarters whole grains or millets, and includes a palm-sized protein. These shifts support steady blood sugar and better lipid profiles without losing traditional flavors or comfort.
4. Cut Refined Carbs and Sugary Drinks

Refined carbohydrates and sugar-sweetened beverages are common drivers of raised triglycerides and insulin resistance. Replacing white bread, white rice, sweetened teas, and packaged sweets with whole grains, lightly sweetened chai, and fresh fruit lowers daily glycemic load. Simple swaps: trade white rice for brown rice or millets a few days a week; replace packaged biscuits with roasted makhana or a small portion of mixed nuts; choose unsweetened yogurt with chopped fruit instead of sugary desserts. Be mindful of drinks: many store-bought juices and bottled beverages carry surprising sugar. Try lime water, unsweetened iced green tea, or plain water infused with slices of cucumber and lemon. When tasting sweets on special occasions, enjoy smaller portions and savor slowly to reduce overeating. Over time, these substitutions can lower fasting triglycerides and fasting glucose, two key metabolic syndrome markers. For many people, gradual changes that keep flavors familiar are easier to sustain than sudden deprivation.
5. Prioritize Sleep and Circadian Health

Quality sleep and a steady sleep schedule matter for metabolic health. Research shows disrupted sleep and shift work are linked with higher metabolic syndrome risk, possibly doubling risk in some shift-worker groups (meta-analysis, 2022). Aim for roughly 7–9 hours each night and a consistent bedtime and wake time, even on weekends. Avoid heavy late-night meals and limit screen time an hour before bed; the blue light and late eating both interfere with circadian rhythm and glucose control. Small habits make a difference: a calming bedtime routine, a cool, dark sleep space, and limiting caffeine after the afternoon help most people fall asleep more easily. If work schedules make a consistent night pattern hard, try to keep a stable sleep window and nap carefully so daytime sleep does not replace restorative night sleep. If you experience persistent insomnia or daytime sleepiness, speak with a clinician — treating sleep apnea or other sleep disorders can meaningfully improve insulin sensitivity and blood pressure.
6. Manage Stress with Simple Tools

Chronic stress raises hormones like cortisol that can worsen insulin resistance and central fat storage. Managing stress doesn’t require long retreat weekends; short, regular practices can help. Try daily breathing exercises (pranayama), five to ten minutes of guided meditation, or a brisk walk during a stressful break. Social connection also buffers stress: a quick phone call to family, a shared evening chai, or community activities supports mental health and resilience. When stress feels overwhelming, brief counseling sessions or talking to a trusted clinician can provide tools that change long-term patterns. Employers and health plans often offer low-cost mental health resources and apps that guide short practices. Simple habit cues — a reminder alarm for a two-minute breathing break, or a walk after a stressful meeting — make techniques sticky. Over weeks, these micro-practices reduce perceived stress and help control behaviors like emotional eating that often follow stress spikes.
7. Feed Your Gut: Fermented and fiber-rich foods

The gut microbiome plays a role in metabolism, and diets that support diverse bacteria are linked with lower metabolic syndrome odds (2025 microbiome research). Focus on fiber diversity — whole grains, pulses, vegetables, fruits, nuts, and seeds — to feed a range of gut microbes. Include fermented traditional foods such as yogurt, idli, dosa, and homemade pickles where safe and not overly salty, as these foods add friendly microbes. A simple daily plate could include a bowl of dal, a vegetable side, a small portion of millet, and a cup of plain yogurt. If you’re new to high-fiber eating, increase fiber gradually and drink more water to ease digestion. Diverse plant foods supply polyphenols and prebiotic fibers which help beneficial bacteria flourish. Supplements can help in some cases, but food-first approaches are generally preferred. If you have digestive symptoms or are immunocompromised, check with a clinician before trying new fermented products.
8. Stop Smoking and Reduce Toxin Exposure

Smoking harms metabolic health by reducing insulin sensitivity and impairing lipid metabolism, and quitting is one of the most powerful moves for long-term risk reduction. Data indicate interactions between inactivity and smoking raise metabolic syndrome risk, so combining cessation with activity is doubly beneficial (Nature/IFM findings). For many households, indoor air quality matters too: choose cleaner cooking fuels where possible and ensure good ventilation to reduce smoke exposure. In urban areas, awareness of outdoor pollution and using masks on high-pollution days can limit inhaled toxins. If quitting feels too big to tackle alone, seek structured support — nicotine replacement, counseling, and local cessation programs improve success rates. Removing ashtrays and asking household members not to smoke indoors both reduce exposure and create a supportive environment. These steps improve lung health, blood pressure, and insulin regulation over time.
9. Keep Meal Timing Consistent

When you eat matters as much as what you eat for metabolic health. Consistent meal timing helps circadian rhythms and insulin patterns; irregular and late-night eating are linked to worse metabolic markers. Aim for a regular eating window — many people find a 10–12 hour window manageable, such as breakfast at 8am and last small snack by 8pm. For shift workers or irregular schedules, try to keep meals at similar clock times relative to your sleep cycle to reduce circadian misalignment. Planning small, balanced meals or tiffin-style portions can reduce the urge to graze on high-sugar snacks. If a full overnight fast feels uncomfortable, start with simple changes: move dinner earlier by 30 minutes or swap late-night sweets for a small portion of fruit. Regular meal timing supports blood sugar stability and makes other changes, like post-meal walking, easier to implement consistently.
10. Use Spices and Whole Foods from Dadi’s Kitchen

Traditional spices and home-cooked meals can support metabolic health when used thoughtfully. Turmeric, cinnamon, and fenugreek are examples of pantry ingredients with bioactive compounds that have modest anti-inflammatory or glucose-modulating effects in research studies. That doesn’t make them cures, but used as part of a balanced diet they add flavour and small potential benefits. Incorporate spices into dals, sabzis, and chutneys instead of relying on packaged seasonings high in salt. Homemade dishes also let you control oil type and portion sizes compared to many processed convenience foods. Try swapping fried snacks for roasted spiced nuts or roasted chickpeas, and use cinnamon in unsweetened yogurt with fruit. These tweaks keep familiar tastes while supporting better glucose and lipid responses across the day. As always, large effects come from overall dietary patterns rather than single ingredients.
11. Include Yoga and Strength Work

Combining yoga with resistance training covers both stress management and muscle-building needs. Yoga promotes flexibility, balance, and lower stress — helpful for blood pressure and mental health — while resistance exercises increase muscle mass and insulin sensitivity. A weekly plan might include two short resistance sessions with bodyweight or light weights and two yoga or mobility sessions to improve recovery and reduce stress. For beginners, simple sun salutations, standing poses, and breathing work form an accessible yoga routine, while chair squats, lunges, and resistance-band rows create a gentle strength plan. Strength training needn’t require a gym; household items like filled water bottles can add resistance. Over months, strength work helps preserve metabolic rate and supports glucose control, while yoga helps sustain the habit by easing soreness and improving sleep. Tailor the mix to your schedule and preferences, and consider a local group class for motivation and instruction.
12. Monitor Key Numbers Regularly

Regular monitoring helps you see progress and catch early warning signs. Track waist circumference, blood pressure, fasting glucose, and fasting lipids at intervals recommended by your clinician. A waist measurement above guideline thresholds signals visceral fat increase, while elevated fasting glucose or triglycerides may indicate metabolic strain. Home blood pressure monitors are affordable and can show trends between clinic visits. If you have risk factors, consider checking fasting glucose and lipid panels annually or as advised by your healthcare professional. Recording results in a simple notebook or phone app makes trends easy to spot and helps you and your clinician adjust plans. When numbers improve, celebrate that success; when they don’t, monitoring makes it easier to discuss next steps like dietary changes, medication, or specialist referral. Good records also help clinicians personalize treatment effectively.
13. Partner with Healthcare Professionals

Lifestyle steps are powerful, but partnering with healthcare professionals ensures safe, effective care tailored to your needs. Primary care doctors, dietitians, certified diabetes educators, and culturally informed practitioners can help set realistic goals, interpret labs, and recommend medications when lifestyle alone isn’t enough. If you have heart disease, diabetes, or multiple risk factors, a stepped plan that combines lifestyle change with medical management lowers risk most effectively. Use visits to discuss blood-pressure or glucose targets, and ask about referral to nutrition services or structured programs. Telehealth or community health centers often offer accessible options if clinic visits are difficult. Bring your food log, activity notes, and monitoring records to visits — concrete data helps clinicians provide concrete advice. A collaborative approach respects your preferences, cultural food choices, and life demands while keeping safety front and center.
Wrap-up: Small steps, big difference
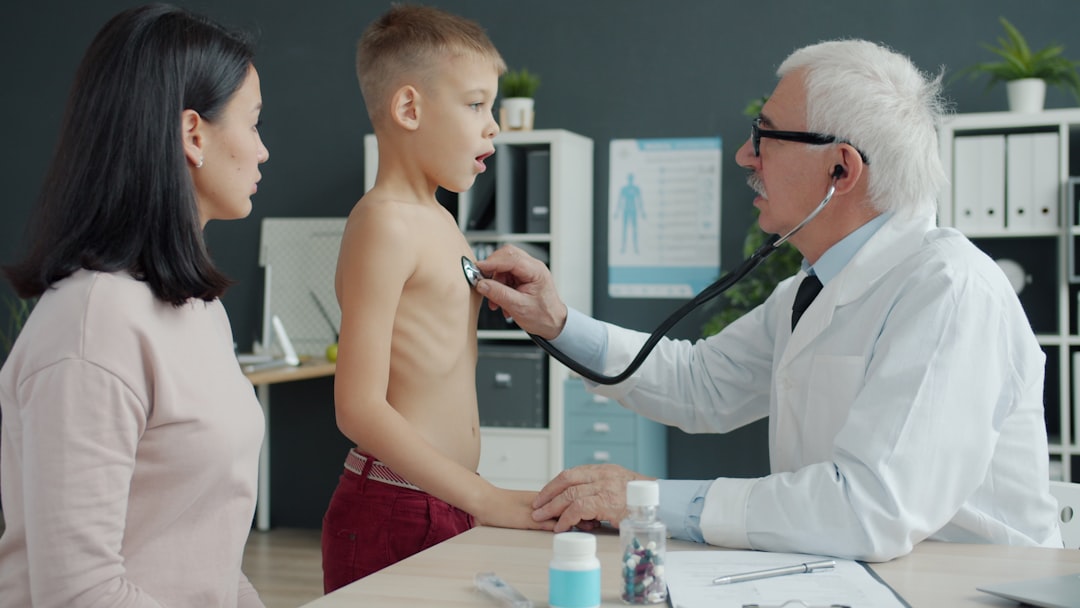
Metabolic syndrome develops from a web of factors, but each step in daily life can pull the web apart. These 13 actions — from adding short walks after meals to choosing whole-grain and vegetable-forward plates, improving sleep, and keeping stress in check — are practical moves you can start this week. Many readers find that pairing two or three changes, such as a nightly post-dinner walk, a swap to brown rice twice a week, and a five-minute breathing practice, creates momentum while remaining doable. Use culturally familiar tools where they help: traditional fermented foods, spices from dadi’s kitchen, and family meal patterns can all be part of a healthy plan. Track progress with simple numbers — waist, blood pressure, fasting labs — and loop in a trusted clinician when needed. Prevention is a team effort that blends daily habits with professional guidance. Start with one habit and build slowly; those small steps compound and lower risk over time. If you have existing medical conditions or take medications, check with your healthcare provider before making major changes. With steady, culturally sensible steps, reducing metabolic syndrome risk is within reach.
