12 Liver Cirrhosis Management Tips to Slow Disease Progression
Living with cirrhosis can feel overwhelming, but there are clear, evidence-based steps that slow damage and reduce risks. This list collects 12 practical management tips tested by hepatology experts and patient-focused resources. You’ll find actions you can take at home—like food swaps for your tiffin or gentle daily movement—and steps your care team will lead, such as surveillance imaging and medication choices. Some causes of cirrhosis can be treated directly, allowing liver function to improve once the harmful factor is removed. Other strategies aim to prevent complications that make life harder, such as fluid buildup, bleeding from enlarged veins, and infections. The goal here is realistic: slow progression, avoid avoidable harm, and keep quality of life high while you work with your doctors. Where traditional remedies come up, I’ll flag safety concerns and point to clinical guidance. The evidence base includes major clinical centers and peer-reviewed work, so readers can trust the recommendations while tailoring them to personal routines and cultural foodways. If you have acute symptoms—confusion, sudden swelling, vomiting blood—seek emergency care right away. Otherwise, use these tips to build a steady plan with your hepatology team and family. Practical steps and timely follow-up make a tangible difference when cirrhosis is managed early and consistently (sources: Mayo Clinic; Rush University; Nature Journal; Apollo247; AMBOSS).
1. Quit alcohol completely

Stopping alcohol is the single most powerful step for anyone whose liver damage stems from drinking. For alcohol-related cirrhosis, complete and lifelong abstinence can halt further injury and sometimes allow partial recovery of liver function. Practical quitting strategies include joining a structured program, seeing an addiction specialist, and using medications when appropriate to reduce cravings. Support can be community-based or clinical; many patients combine peer groups with medical follow-up. In Indian families, social rituals often involve alcohol; make a plan with family members to avoid triggers at festivals or social gatherings and keep nonalcoholic substitutes ready. If withdrawal is likely, get medical help—sudden stopping after heavy use can be dangerous without supervision. Your care team can connect you to culturally sensitive resources, such as counselors who understand local drinking patterns and community support groups. Expect setbacks; the focus should be on progress rather than perfection. When alcohol is removed, other treatments—like antiviral drugs or weight-loss measures—work better and faster, giving the liver a chance to heal. (Sources: Apollo247; Rush University.)
2. Treat the root cause promptly
Slowing cirrhosis starts with addressing what caused it. If hepatitis B or C is to blame, antiviral medicines can suppress the virus and reduce ongoing damage. For metabolic-related liver disease (often called MASH or MAFLD), the focus is on weight, blood sugar, and cholesterol control. Autoimmune liver diseases, uncommon but serious, need immune-directed medications. Early diagnosis lets specialists tailor treatment that can stabilize or improve liver health. Working with a hepatologist helps you prioritize tests and treatments; many centers now offer coordinated clinics that combine nutrition, diabetes care, and counseling under one roof. In practice, this means keeping appointments, sharing complete medical histories, and asking your team about targeted therapies. Some treatments require monitoring—blood tests, imaging, and sometimes liver biopsies—so organize your records and set reminders. Treating the cause doesn’t replace lifestyle steps, but it often amplifies their benefits. Discuss medication options, expected timelines, and monitoring plans with your provider so you and your family can make informed choices that fit your daily life and cultural routines.
3. Follow a liver-friendly diet with practical Indian swaps

Food matters. A liver-friendly diet helps control fat buildup, supports recovery, and reduces complication risks. Focus on whole foods: vegetables, whole grains, legumes, lean proteins, and healthy fats like mustard or olive oil in modest amounts. Limit refined sugars, white flour, and fried snacks that pack calories without nutrition. For readers used to tiffins, swap deep-fried samosas for baked vegetable cutlets, choose brown rice or millets over polished white rice sometimes, and add a bowl of dal or chana for protein. Portion control is more important than eliminating beloved foods—use smaller plates and share sweets during family gatherings. For people with fluid retention, also pay attention to sodium (see tip 4). If you have diabetes or high cholesterol alongside cirrhosis, coordinate with a dietitian who can create an individualized plan that respects regional preferences. Traditional spices—turmeric, coriander, cumin—can add flavor with little calorie cost; curcumin has anti-inflammatory interest, but don’t assume herbal remedies are safe for the liver without checking with your doctor. A registered dietitian or hepatology nurse can help you draft a weekly meal plan that fits your palate and medical needs.
4. Control salt and fluids to manage ascites

Fluid accumulation in the belly (ascites) is common in cirrhosis and responds well to routine salt and fluid management paired with medical treatment. Your provider may recommend a sodium goal—often around 2 grams per day, though recommendations vary—so learn to read labels and prepare low-salt versions of favorite dishes. Small swaps help: rinse canned vegetables, use fresh herbs for flavor, and avoid ready-made spice mixes high in salt. Weigh yourself daily at the same time to catch rapid weight gain that signals fluid retention. If swelling increases, your clinician may add or adjust diuretics; follow dosing closely and report dizziness or extreme thirst. In the home setting, elevate legs and sleep with a slight incline if needed to ease breathing when fluid is heavy. Avoid self-adjusting diuretics or diet extremes; too-rapid fluid loss can harm kidneys and other organs. Consistent daily monitoring—food choices, salt checks, and weight logs—lets your team fine-tune medical therapy and prevent hospital visits.
5. Keep protein adequate and aim for steady weight

Contrary to older beliefs, most people with cirrhosis need adequate protein to prevent muscle loss and weakness. Aim for steady daily protein intake from pulses, low-fat dairy, eggs, and lean fish or poultry depending on dietary habits. For vegetarian diets common across Indian households, include a variety of dals, paneer in moderation, and soy or legume mixes in tiffins. Avoid extreme protein restriction unless your care team prescribes it temporarily for acute problems. Muscle mass helps the body handle infections and complications, and keeping strong reduces falls and frailty. If weight loss is advised, aim for a gradual pace—around half a kilogram to one kilogram per week—so the liver and kidneys tolerate the change. Those managing obesity-related liver disease benefit from modest weight loss, which often reduces liver fat and inflammation. Work with a dietitian and your hepatology team to set clear protein and calorie targets and adapt them to cultural meal patterns and household routines.
6. Exercise safely to build strength and metabolic health

Regular, moderate exercise helps control weight, improves insulin sensitivity, and preserves muscle—important goals for slowing cirrhosis progression. Combine daily brisk walking, cycling, or easy aerobic classes with two resistance sessions per week that focus on major muscle groups. For many readers, simple routines fit family life: a 30-minute brisk walk after the evening tiffin or bodyweight exercises during short breaks. If you’re new to activity or have fluid or heart concerns, check with your care team before starting. Yoga and gentle stretching can improve balance and reduce stress; choose poses that match your strength level and avoid breath-holding maneuvers if you have ascites or severe portal hypertension. Keep sessions consistent and track progress: small increases in walking time or an extra set of squats count as wins. Physical activity improves mood and sleep too, helping you stick to other lifestyle goals that support liver health.
7. Take medicines correctly and avoid hepatotoxic substances

Medication safety matters more with cirrhosis because the liver processes many drugs. Keep an up-to-date medication list and use a pill organizer or app to avoid missed doses. Ask your clinician or pharmacist before starting any new prescription, over-the-counter drug, or herbal supplement. Common nonsteroidal anti-inflammatory drugs (NSAIDs) and some herbal remedies can worsen bleeding risk or damage kidneys in cirrhosis and are often safer to avoid. Your provider may prefer acetaminophen at low doses for pain instead of NSAIDs, but always confirm a dose that’s safe for you. Herbal supplements marketed for liver health can be unpredictable; some cause harm, so do not self-prescribe them. If a medication requires liver monitoring, schedule and track blood tests; early lab shifts often guide dose changes that prevent complications. Clear communication between you, your primary care provider, and hepatology reduces dangerous interactions and keeps treatment goals on track.
8. Monitor regularly and stick to surveillance schedules
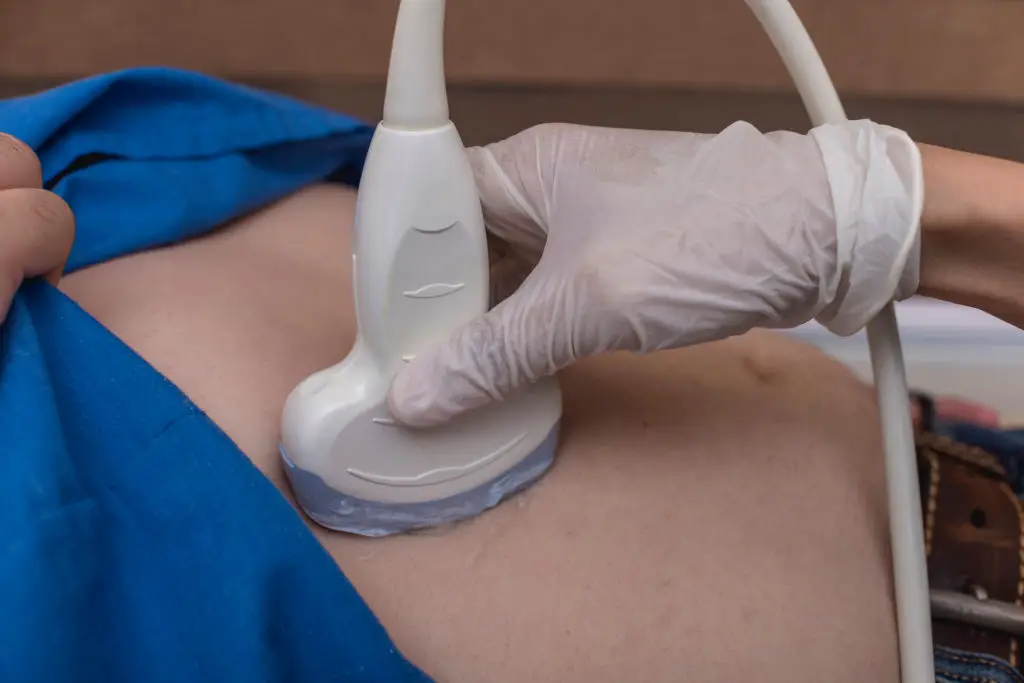
Routine monitoring is a cornerstone of cirrhosis care because early detection of changes allows timely action. Typical follow-up includes blood tests to check liver enzymes, albumin, bilirubin, and clotting status, along with ultrasound imaging every six months in many patients to screen for liver cancer. If portal hypertension is suspected, your team may recommend periodic endoscopy to check for varices. Keep a calendar of these appointments and get copies of test results to track trends. If results shift, the care team can intervene—adjusting medications, ordering additional imaging, or scheduling procedures—to prevent emergencies. In busy households, assign a family member to coordinate visits and prescriptions; in Indian families, this often means a close relative or dadi managing appointments. Telehealth follow-ups can help when travel is hard, but make sure essential tests are still done in person. Regular surveillance saves lives by catching treatable problems early.
9. Prevent infections with vaccines and early treatment
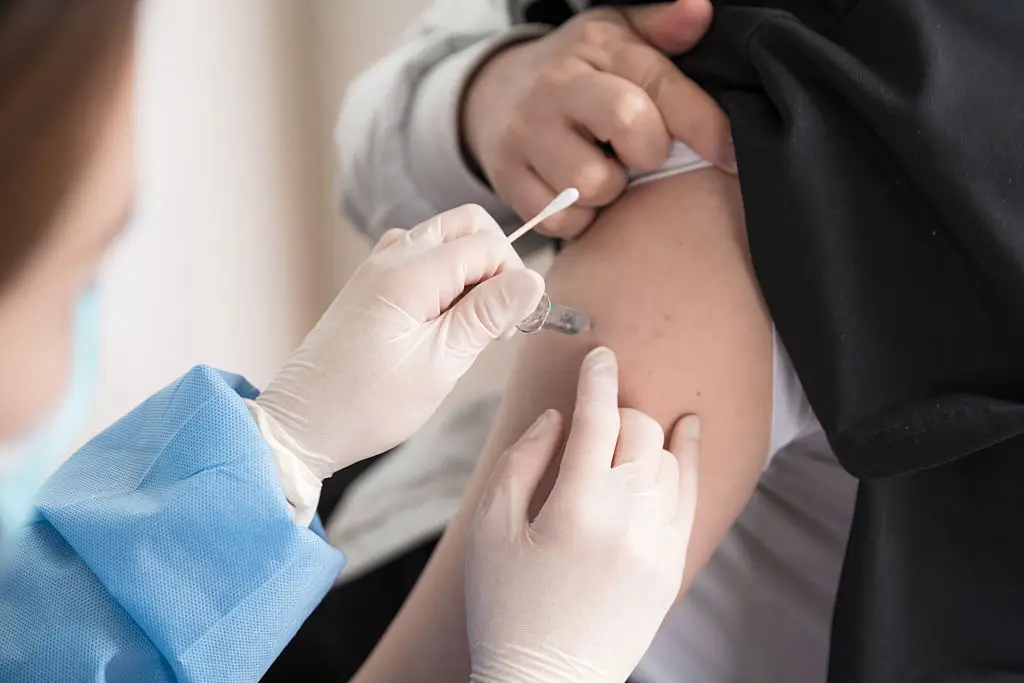
People with cirrhosis are more vulnerable to infections, and preventing them reduces hospital stays and complications. Make sure vaccinations are up to date: hepatitis A and B if susceptible, annual influenza, and pneumococcal vaccines as recommended by your doctor. Discuss shingles and COVID-19 boosters based on your age and health. Simple hygiene—handwashing, safe food handling, and prompt dental care—also lowers infection risk. If you develop fever, cough, or urinary symptoms, contact your provider early; infections can worsen liver function quickly. For travelers or family events, talk to your care team about additional precautions. When antibiotics are prescribed, take the full course as directed, and notify clinicians if symptoms worsen. Vaccination and quick treatment of infections are practical steps with high impact on keeping cirrhosis stable.
10. Manage portal hypertension and variceal risk
Portal hypertension—the high pressure in veins leading to the liver—causes dangerous varices that can bleed. Proactive management reduces that risk. If screening endoscopy shows large varices, your hepatologist may recommend nonselective beta-blockers or endoscopic band ligation to prevent bleeding. Learn to spot warning signs—black or bloody stools, vomiting blood, or sudden fainting—and seek emergency care immediately if they occur. Avoid activities or medications that raise bleeding risk unless advised by your clinician. For people with varices, regular follow-up endoscopies and adherence to medication are crucial. Families should also know basic first-aid and emergency contacts in case of bleeding. Working with a specialist center makes these preventive steps more accessible and effective, and when combined with lifestyle measures they markedly reduce life-threatening events.
11. Support mental health and build a care team

A cirrhosis diagnosis impacts mood, sleep, and daily roles; addressing mental health is part of good liver care. Depression and anxiety affect self-care tasks—medication adherence, diet, and clinic follow-up—so seek counseling early if you notice persistent low mood or withdrawal. Peer groups and structured addiction support help with recovery and long-term planning. In many households, family support—simple tasks like preparing low-salt meals or reminding about medicines—makes a measurable difference. If language or cultural barriers exist, request culturally sensitive counseling and community resources. Social workers can assist with insurance, transport, and disability concerns, while palliative teams help manage symptoms when the focus shifts from cure to comfort. A strong care team combines medical, nutritional, and psychosocial support so you and your family face cirrhosis together rather than alone.
12. Discuss transplant evaluation early and coordinate long-term care

For some people with progressive cirrhosis, liver transplant offers the best long-term outcome. Discussing transplant evaluation early does not mean immediate need; it simply opens options and lets teams optimize health ahead of time. Referral to a transplant center triggers detailed assessment—medical, surgical, and psychosocial—that prepares you for each step if needed. Even if transplant isn’t the final path, the evaluation clarifies prognosis and supports advanced care planning. Coordinate primary care, hepatology, and transplant teams so medications, vaccinations, and lifestyle steps align with transplant goals. If transplant is not appropriate, palliative care still provides symptom relief, hospice planning, and family support. Early conversations ease later decisions and let you focus on goals that matter to you and your loved ones.
Final thoughts: steady steps add up

Cirrhosis can be serious, but many measures slow its course and reduce crises when applied consistently. The most impactful steps are within reach: stop alcohol, treat what caused the damage, eat well with culturally familiar swaps, control salt and fluids, maintain protein and strength, get vaccinated, and keep up with monitoring and specialist care. Avoid unsafe medications and unverified supplements, and reach out for mental-health or addiction support when needed. These actions work best when coordinated with a hepatology team and family members who help with day-to-day routines—whether that’s preparing a balanced tiffin or tracking clinic appointments. Set small, measurable goals: one tobacco- or alcohol-free festival, a weekly walking plan, regular lab checks on the calendar. Keep copies of tests and ask your providers for a clear follow-up schedule. If symptoms escalate, seek care promptly—many emergencies are avoidable with early action. Use the trusted sources below to guide conversations with clinicians and share this plan with caregivers so everyone knows the priorities. With steady, practical steps and reliable medical follow-up, people with cirrhosis can preserve quality of life and slow disease progression.
