11 Doctor-Recommended Women's Health Screening Tests You Should Know
Preventive health screenings are one of the simplest ways to catch issues early and protect long-term wellbeing. Doctors and major medical groups agree that regular tests — timed to your age, health history, and risk factors — reduce the chance of surprise diagnoses and help guide treatments that keep you active and working. This guide pulls together doctor-recommended screenings that most clinicians talk about during a well-woman visit: cervical and breast cancer checks, colon cancer screening, bone density tests, cardiovascular and diabetes checks, skin and sexual-health testing, sensory screenings, genetic evaluation for high-risk families, and targeted hormone or thyroid testing when symptoms appear. Think of this list as a starting framework rather than a strict schedule. Your clinician will tailor timing and frequency based on family history, past results, and lifestyle. If your dadi told you to watch your weight, she was passing along a real risk-management tip: many screening choices link to modifiable risks like smoking, alcohol, diet, and exercise. Use this checklist to prepare questions for your next visit: ask about age-based timing, any prep you need, and what abnormal results usually mean. Finally, if cost or insurance is a concern, bring that up during scheduling — many preventive services are covered under US insurance plans. Regular screening isn’t one-size-fits-all, but staying informed and booked is a reliable way to stay healthy.
1. Cervical Cancer Screening (Pap and HPV tests)
Cervical screening saves lives by catching precancerous cell changes before they turn invasive. Doctors advise beginning Pap tests at age 21. For ages 21–29, a Pap every three years is a standard approach for most women without symptoms. At age 30 through 65, clinicians often recommend either a Pap every three years or HPV co-testing every five years. HPV testing screens for the virus types most linked to cervical cancer and can lengthen safe intervals between checks. If a Pap or HPV result is abnormal, follow-up might include a repeat test, colposcopy, or biopsy to pinpoint the issue. Practical tips help: schedule your appointment when you are not menstruating, avoid douching and intercourse for 24–48 hours before the test, and bring prior records so providers can compare results over time. For women who have had a hysterectomy, screening guidance depends on why the surgery was done and whether the cervix was removed. Talk with your gynecologist about vaccination status, previous abnormal results, and any bleeding or unusual symptoms. Staying current with cervical screening cuts the odds of advanced disease and keeps follow-up options simpler.
2. Breast Cancer Screening (Mammograms)
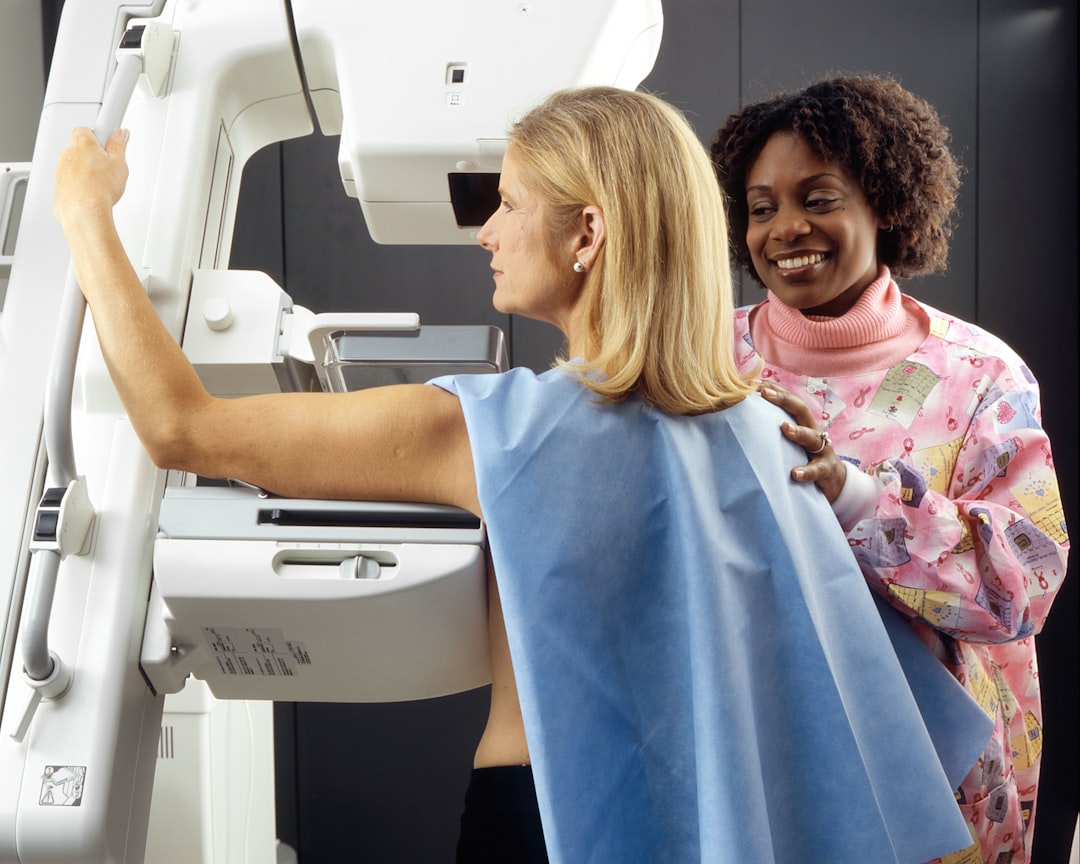
Breast cancer screening detects lumps or microcalcifications before they cause symptoms. Many doctors recommend starting conversations about routine mammograms at age 40, with shared decision-making guiding frequency. Some clinicians suggest annual screenings for average-risk women, while others may recommend every two years based on personal risk and prior imaging. Women with dense breasts often benefit from 3D mammography or additional imaging, which improves detection in dense tissue. If you have a strong family history or genetic risk, your care team may start imaging earlier or add MRI. Practical prep includes avoiding deodorant, powders, or lotions on the day of the test and bringing previous mammogram images to help radiologists compare. A normal report typically returns to routine screening. If radiologists find something unusual, they may request diagnostic mammography, ultrasound, or a biopsy to determine whether the finding is benign or cancerous. Remember that early detection usually means simpler treatment and better outcomes, so discuss your individual risk and screening schedule with your clinician.
3. Colorectal Cancer Screening (Colonoscopy and alternatives)
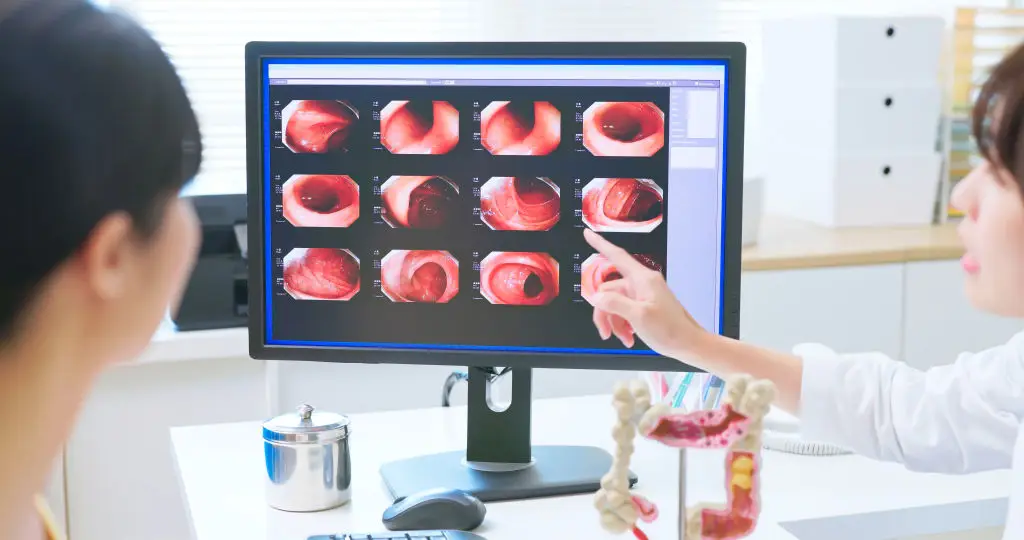
Colorectal cancer screening looks for polyps and early cancers that usually have no symptoms. Current guidelines recommend starting screening at age 45 for average-risk adults. Colonoscopy every ten years is the standard option because it both finds and removes polyps, but stool-based tests such as FIT or stool DNA screens offer non-invasive alternatives that are done yearly or every few years depending on the test. If a test finds polyps, follow-up intervals shorten based on polyp type and number. Bowel prep is required for colonoscopy and is often the most important part of a successful test; follow instructions carefully for a clear exam. Discuss family history and any gastrointestinal symptoms with your provider, because a personal or family history of polyps or colorectal cancer can mean earlier or more frequent screening. If someone in your family had colorectal cancer at a young age, your clinician may suggest genetic counseling or earlier colonoscopy. Catching polyps early prevents cancer and saves lives.
4. Bone Density Screening (DEXA scan)
Bone density testing measures the strength of your bones to assess osteoporosis risk and fracture chance. For average-risk women, many guidelines recommend starting DEXA screening at age 65. Women with risk factors — a thin body frame, long-term steroid use, smoking, low calcium intake, or a family history of fractures — may start screening earlier, often around age 50. The test is quick and painless: you lie on a table while the scanner measures bone density at the hip and spine. Avoid taking calcium supplements right before the test unless your clinician tells you otherwise. Results are reported as T-scores that compare your bone density to a healthy young adult; lower scores indicate weaker bones and may prompt lifestyle changes, supplements, or medications to reduce fracture risk. If you’ve had a fracture after age 50, ask your doctor about testing sooner. Strong bones support mobility and independence, making screening an important part of long-term health planning.
5. Cardiovascular Screening (Lipid Panel and Risk Assessment)
Heart disease is a leading cause of death among women, and regular cardiovascular screening helps spot risk early. A baseline lipid panel — measuring total cholesterol, LDL, HDL, and triglycerides — is commonly done in early adulthood and repeated every four to six years for those at average risk. If you have diabetes, high blood pressure, a family history of premature heart disease, or tobacco use, clinicians recommend more frequent testing and a fuller risk assessment. Some providers now add advanced markers such as lipoprotein(a) or apolipoprotein B when family history or prior results suggest higher residual risk. Fasting may be requested for certain lipid tests, so confirm prep when scheduling. Results guide lifestyle advice and, for many people, medication decisions to lower LDL and reduce cardiovascular risk. Combining cholesterol data with blood pressure, weight, and smoking status gives a clearer picture of heart health and helps clinicians personalize prevention.
6. Diabetes Screening (Hemoglobin A1c)
Diabetes screening detects elevated blood sugar before serious complications begin. Hemoglobin A1c shows average blood glucose over the previous two to three months and is a commonly used screening tool. Many clinicians recommend starting screening around age 35 for people at average risk, while those with obesity, a family history of diabetes, previous gestational diabetes, or other risk factors should be tested earlier and more often. If an A1c is in the prediabetes range, lifestyle changes like modest weight loss and increased activity often reduce progression to type 2 diabetes. No special prep is usually required for an A1c, though some labs may prefer fasting for other related tests. Results fall into normal, prediabetes, and diabetes categories, and each bracket has an action plan from watchful waiting to medication and referral to diabetes education. Early detection gives more options to prevent complications like nerve damage or heart disease.
7. Skin Cancer Screening (Dermatology exam and self-checks)

Skin checks are a practical way to catch melanoma and other skin cancers early, when treatment is most successful. Self-exams are simple: once a month, look for new moles, spots that change shape, color, or size, and anything that bleeds or won’t heal. Dermatologists often recommend annual full-body skin exams for people with many moles, a personal or family history of skin cancer, or significant sun exposure. If you have fair skin, a history of tanning-bed use, or frequent sunburns, be extra vigilant. During a clinic exam, photographers or dermoscopy tools may be used to document suspicious lesions. A biopsy is the definitive test if a mole looks abnormal. If caught early, most skin cancers are highly treatable. Protect your skin with sunscreen, protective clothing, and by avoiding peak sun hours.
8. Sexual Health Screening (STD testing)
Sexually transmitted infection screening is essential because many STDs are symptomless but can cause serious problems if untreated. Doctors recommend routine testing for sexually active women, with special emphasis on younger adults and anyone with new or multiple partners. Chlamydia and gonorrhea screening is commonly recommended annually for sexually active women under 25, and more often if there are new risk factors. Tests are usually quick swabs or urine samples, and treatment is straightforward for most bacterial infections. Pregnant women undergo specific screening to protect the baby, and clinicians discuss HIV, syphilis, hepatitis, and HPV vaccination as part of comprehensive care. Being open about sexual history helps your provider pick the right tests. Early detection prevents complications and stops transmission to partners.
9. Vision and Hearing Assessments

Good vision and hearing are central to daily life, work, and safety, so routine checks matter. Eye exams every two years are common for adults under 60; after 60, many clinicians recommend annual eye exams to monitor age-related conditions like cataracts or macular degeneration. Hearing assessments are often done less frequently for younger adults but become more regular after age 50 or with symptoms such as trouble following conversations. Tests are simple: vision exams use charts and lenses, while hearing checks use audiometry to measure frequencies and thresholds. Bring current glasses or hearing aids to appointments. Early changes can be addressed with corrective lenses, hearing devices, or referrals to specialists. Managing sensory health supports mental sharpness and social engagement, so don’t delay scheduling when you notice changes.
10. Genetic Cancer Screening (BRCA and panel testing)
Genetic testing looks for inherited mutations that raise the risk of cancers such as breast and ovarian cancer. Doctors recommend considering genetic testing if you have a strong family history of early-onset breast, ovarian, pancreatic, or related cancers, or multiple affected relatives across generations. If family history suggests elevated risk, clinicians usually refer patients to genetic counseling before testing so you understand implications for screening and prevention. A positive test can change screening timelines — for example, earlier mammography, supplemental MRI, or even preventive surgery may be discussed — and it also informs family members who might carry the same mutation. Testing is done with a blood or saliva sample, and insurers often require documentation of medical necessity. If you’re unsure about whether family history rises to the level of testing, start the conversation with a primary care doctor or genetic counselor to map next steps.
11. Hormone and Thyroid Screening (When symptoms warrant)

Hormone and thyroid testing aren’t one-size-fits-all routine screens. Instead, clinicians order these tests when symptoms suggest imbalance — irregular periods, hot flashes, unexplained fatigue, weight changes, or mood shifts. Thyroid-stimulating hormone (TSH) is a common first test for suspected thyroid dysfunction, which can mimic or worsen other health issues. For perimenopause and menopause concerns, doctors may check FSH, estradiol, or other markers in the context of symptoms and age; however, clinical decisions often rely more on symptoms than single lab values. Bring a complete medication list to tests because some drugs affect hormone levels. Results guide targeted treatment: thyroid hormone replacement, short-term symptom management, or lifestyle strategies for menopausal symptoms. Because screening is individualized, ask your clinician whether testing makes sense based on your symptoms and personal history.
Wrap-up: Build a personalized screening plan with your clinician

Screening is most effective when tailored to you. This checklist covers 11 doctor-recommended tests that commonly arise during well-woman visits, along with practical tips on timing, preparation, and what abnormal results can mean. Use it as a conversation starter rather than a rigid schedule. Your age, family history, race, medical conditions, and lifestyle shape the right plan. For example, family history might prompt earlier genetic testing or colorectal screening, while denser breasts may call for supplemental imaging. If cost is a worry, ask clinic staff about billable preventive benefits — many insurers cover recommended screenings. Keep records of past tests and bring them to appointments; that simple step helps doctors compare trends and avoid unnecessary repeats. Finally, regular screening pairs with everyday care: balanced meals, physical activity, and stress management help lower risks across many conditions. Book a well-woman visit, prepare your questions, and bring up any symptoms you’ve hesitated to mention. A small bit of planning now gives you better odds of staying healthy and active for the years ahead.