11 Neurological Disorder Facts Everyone Should Know
Neurological disorders quietly touch far more lives than most of us expect. A 2025 Yale analysis reported that conditions affecting the nervous system now impact about 54 percent of people in the United States, a startling figure that points to a hidden burden across families and communities (Yale News, 2025). That number includes a wide range of conditions — from epilepsy and migraines to stroke and degenerative diseases like Alzheimer’s — and many of these start with subtle signs that are easy to miss. Think of how dadi might notice small changes at the tiffin table or a neighbour might mention forgetting a name: these everyday cues can sometimes point to something deeper. This article pulls together eleven reliable, practical facts that everyone should know, mixing clear statistics with simple actions you can take at home or in your community. Each item explains why the fact matters, what to watch for, and one or two things you can do right away. Whether you’re supporting an older relative, teaching a young caregiver, or just trying to be prepared, these facts aim to turn worry into helpful steps. Sources include Yale, the Epilepsy Foundation, Mayo Clinic, WHO, CDC, and medical reviews on neuroplasticity. Read on to learn key signs, bust common myths, and find practical ways to help someone who needs support today.
1. The scale is bigger than you probably think: neurological conditions affect over half of Americans

The latest research shows this is more common than most people realise. A 2025 study reported about 54 percent of the U.S. population has a condition affecting the nervous system, which translates to roughly 180 million people living with a neurological issue (Yale News, 2025). That includes chronic conditions like epilepsy, migraine, stroke-related problems, and nerve damage from diabetes. Many of these problems cause long-term disability rather than immediate death, and that changes how families manage work, childcare, and daily routines. Dr. John Ney at Yale has pointed out that people often ignore early warning signs such as sudden weakness or persistent numbness, and by the time they act the window for preventing lasting harm can be missed (Yale News, 2025). For a practical takeaway, keep an eye out for gradual changes in memory, coordination, or sensation in loved ones; these may be subtle but worth a clinic visit. A neighbour, family member, or local community health worker who notices habits changing early can make a real difference by encouraging timely medical evaluation.
2. Epilepsy is common — and basic seizure first aid saves lives

Epilepsy affects many families and often comes with myths that make people nervous. About one in 26 people will develop epilepsy at some point in their life, and at least a million Americans have seizures that are not fully controlled by medication (Epilepsy Foundation, 2025). A few practical rules make a big difference during a seizure: stay calm, keep the person safe from hard edges, and gently roll them onto their side once jerking stops — the simple “Stay, Safe, Side” approach helps reduce injury. Never try to put anything in someone’s mouth — people cannot swallow their tongue during a seizure, and forcing objects can cause injury (Mayo Clinic). If the seizure lasts more than five minutes, if another seizure follows immediately, or if the person does not wake normally, call emergency services. Families can prepare by learning local first-aid guidance, keeping emergency contact details handy, and talking with doctors about seizure action plans. Small practical steps at home, like securing sharp edges in a kitchen or tiffin area, can reduce risk for people who have frequent seizures.
3. Recognise a stroke quickly: FAST can prevent long-term disability

Time matters with strokes in a way most conditions do not. Use the FAST check: Face drooping, Arm weakness, Speech difficulty, Time to call emergency services. When care happens quickly, treatments such as clot-busting medication can reduce long-term disability and improve recovery odds (CDC). Some people assume a headache or dizziness will pass on its own, but sudden onset of weakness, numbness, trouble speaking, or visual disturbances needs immediate attention. Dr. Ney highlights that ignoring early warning signs can lead to avoidable, long-term problems (Yale News, 2025). If you see these symptoms, do not wait to call 911 — minutes count. For caregivers, keeping a simple note with medication lists and a nearby phone can speed care. In workplaces and community centers, a short poster with FAST reminders can help neighbours act fast if a stroke happens nearby.
4. Memory loss isn't always dementia — but getting assessed matters for care

For many families, the word “forgetfulness” triggers a lot of worry. Mild memory lapses are part of normal aging, but persistent problems with daily tasks, language, or recognizing close relatives suggest a medical assessment. Alzheimer’s and other dementias have varying patterns: some begin with short-term memory loss, while others start with language or planning difficulties. Early diagnosis allows families to plan practical routines, connect with support services, and begin treatments that can manage symptoms and improve quality of life. Care strategies that help include simplifying daily steps like one-pot meal prep or labelled tiffin containers, establishing predictable routines, and using memory aids such as calendars and photos. If behavior changes suddenly, or if someone becomes easily lost in familiar places, seek evaluation sooner rather than later. Support groups, respite care options, and community resources can relieve family stress and improve consistency of care over time.
5. Parkinson’s signs can be subtle at first — small changes in movement matter

Parkinson’s disease often starts with subtle movement changes that families dismiss as age. Common early signs include a resting hand tremor, a softening voice, slowness of movement, and stiffness. These symptoms slowly interfere with daily tasks like buttoning a kurta or opening a tiffin — and practical home changes can help maintain independence. Exercise and physical therapy improve mobility and balance, while occupational therapy suggests simple tools and routines that ease tasks at home. Medications can reduce symptoms for many people, and neurologists can advise on personalized plans. If you notice someone shuffling, losing facial expression, or having difficulty with fine motor skills, it’s time for a clinical review. Family involvement in keeping an encouraging, structured environment and joining movement classes can have a real positive impact on daily living.
6. Multiple sclerosis often begins with subtle neurological symptoms
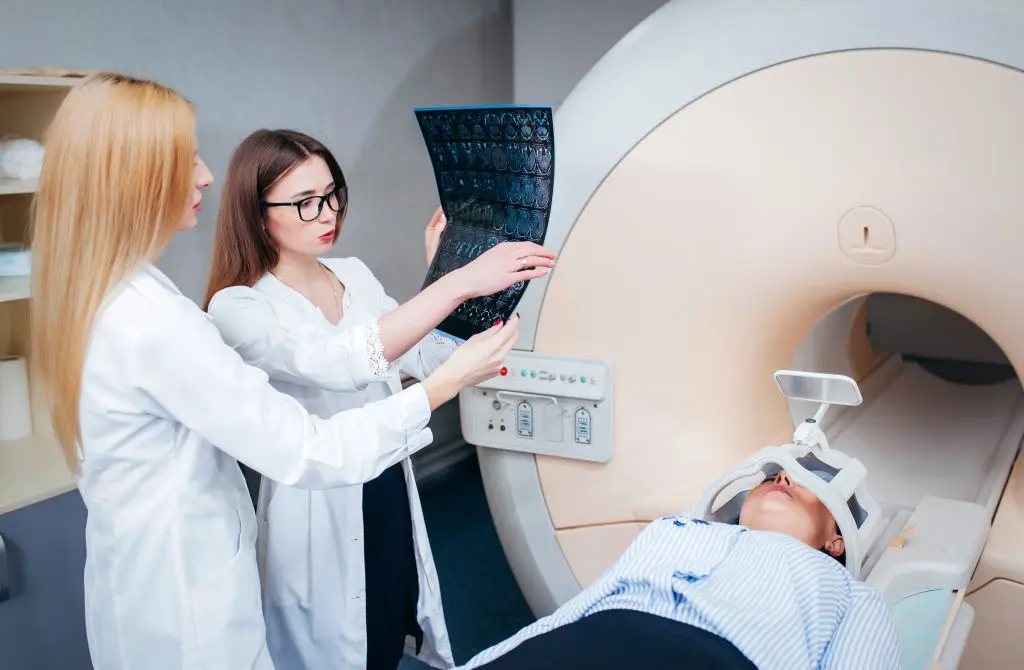
Multiple sclerosis, or MS, commonly starts in young to middle adulthood with symptoms that come and go. Early signs can include blurred vision, numbness or tingling in a limb, trouble with balance, and unusual fatigue. Because symptoms can appear and then improve, people sometimes delay seeking care, which can slow access to disease-modifying treatments that reduce relapses. MRI and specialist evaluation are typical parts of diagnosing MS, and early engagement with a neurologist gives the best chance to design a treatment plan. For day-to-day life, a structured routine, energy-conserving strategies like pacing activities, and assistive devices when needed make tasks easier. Families can help by tracking symptom patterns and sharing them with clinicians, since clear records often speed diagnosis.
7. Not every bad headache is a migraine — know the red flags

Headaches are extremely common, but some types need urgent attention. Migraines often come with throbbing pain, sensitivity to light, nausea, and sometimes visual aura. However, sudden “worst-ever” headaches, headaches after head injury, or headaches with fever and neck stiffness can signal dangerous conditions like bleeding or infection and require urgent evaluation. Keeping a headache diary that notes timing, triggers, duration, and associated symptoms helps clinicians find the right diagnosis and treatment. Lifestyle steps such as regular sleep, hydration, and mindful use of tiffin-time caffeine can reduce frequency for many people. If new headache patterns emerge, or if over-the-counter medicines stop working, seek medical advice to avoid preventable complications and to get treatment recommendations tailored to the person’s life and routine.
8. Peripheral neuropathy is common in diabetes — protect feet and act early
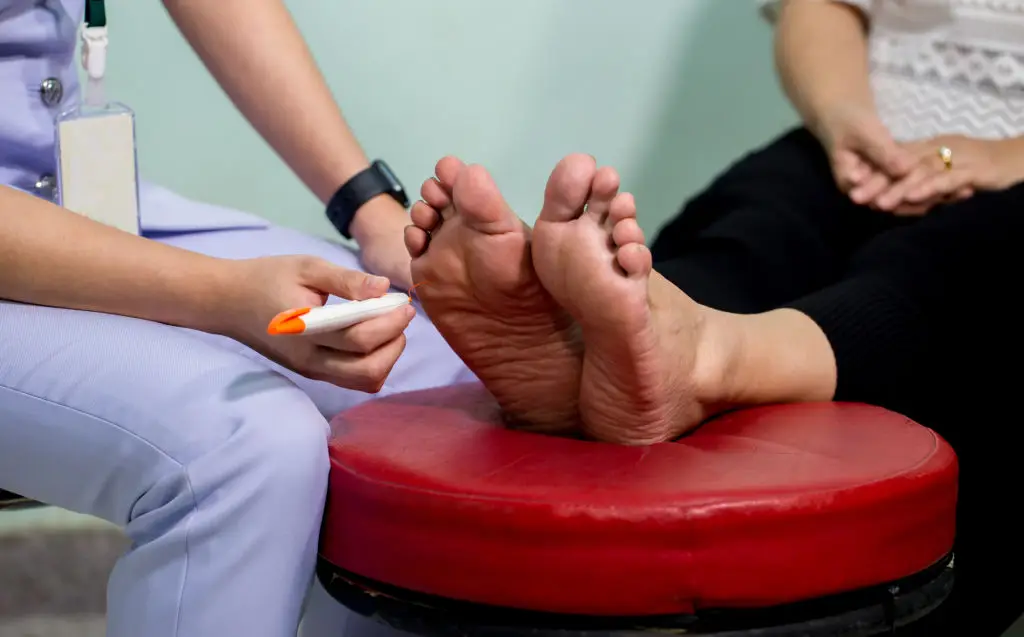
Nerve damage in the feet and hands — peripheral neuropathy — is a frequent complication of diabetes and causes numbness, burning, or sharp pain. When sensation is reduced, small cuts and sores can go unnoticed, increasing the risk of infection and more serious problems. Daily foot checks, good footwear, and regular blood sugar control are the best early defenses. Healthcare teams can offer footcare education and screening that prevents small issues from becoming major problems. If someone describes burning sensations, constant numbness, or balance problems, encourage a check with a clinician and ask about referral to specialists for nerve testing or pain management. Community screening programs and simple at-home checks are practical ways for families to stay ahead of complications.
9. Concussion and TBI can have delayed effects — watch for changes over days and weeks

A blow to the head may seem minor at first but cause lasting problems if unmanaged. Symptoms of concussion include headache, confusion, dizziness, and trouble concentrating, and some people develop sleep problems or mood changes days later. Children and athletes often under-report symptoms, so careful observation and a gradual, supervised return to activity are important. Medical guidance usually recommends rest at first, followed by a staged return to normal activities under clinician supervision. If someone has prolonged headaches, repeated vomiting, worsening confusion, or new neurological signs, seek immediate imaging and specialist care. Keep a simple symptom log for the first two weeks after an injury; it gives clinicians a clear picture and helps families decide when to escalate care.
10. Early signs of autism matter — screening opens doors to helpful supports

Autism spectrum disorders show up early in development, but signs are not always obvious at first. Warning flags include delayed speech, limited eye contact, repetitive behaviors, and difficulty with social responses. Early screening through pediatric visits leads to earlier access to therapies that improve communication and daily skills. Families benefit from community resources and culturally sensitive support that respect home languages and caregiving traditions. For example, incorporating routine social games at mealtime or adapting play to local customs can make interventions feel practical and natural. When concerns arise, ask a pediatrician about developmental screening and early intervention resources; early, consistent support often changes long-term outcomes for the better.
11. The brain adapts — simple daily habits support neuroplasticity at any age

Neuroplasticity means the brain can form new connections throughout life, which is good news for recovery and maintenance. Research shows activities like regular aerobic exercise, quality sleep, learning new skills, and social engagement support healthy brain networks (VeryWell Mind; medically reviewed). Even small daily steps — a short walk after a meal, trying a new recipe in the kitchen, learning a language phrase each week, or playing board games with family — stimulate the brain. For those recovering from injury or managing chronic conditions, structured rehabilitation programs and consistent routines enhance outcomes. Families can support brain health by encouraging gentle activity, varied mental tasks, and steady sleep habits. These are simple, practical habits that fit into everyday life and help the nervous system stay resilient.
Wrap-up: Awareness leads to better action — practical steps you can take now

Neurological conditions affect a surprisingly large share of people, and that scale makes awareness essential for families and communities. Knowing core facts — the prevalence of nervous-system disorders, basic seizure first aid, how to spot stroke signs, and the difference between routine forgetfulness and dementia — lets you act sooner and avoid preventable disability. Small, everyday practices matter: keep emergency numbers handy, learn simple first-aid steps, track new or changing symptoms, and encourage routines that support brain health like exercise and sleep. If you come from a household where dadi’s tips are part of daily care, blend that wisdom with medical guidance: enjoy haldi doodh for comfort but seek care promptly for persistent or worsening symptoms. For caregivers, create predictable routines like labelled tiffin boxes or photo cue cards to reduce stress and improve daily life. Use trusted sources such as Yale’s analysis, the Epilepsy Foundation, Mayo Clinic, WHO, and CDC when making decisions or seeking care. When in doubt, a timely clinical evaluation can be the difference between quick recovery and a long-term problem. Awareness plus simple action helps people live better, safer lives—and it makes communities stronger.