11 Reproductive Health Facts from India and Beyond That Need More Awareness
India's reproductive health story is richer and more complex than headlines suggest. Some changes are quietly positive, like falling maternal deaths in many states, while others remain hidden: low screening for cervical cancer, gaps in contraceptive counseling, and stigma around infertility. This piece brings together 11 facts drawn from research and frontline programs, with eight items rooted in India’s experience and three that explain what those lessons mean for North America and global health. The Best Search Results voice here aims to be like a helpful neighbor — straightforward, culturally aware, and practical. Imagine the kind of advice your dadi might give, paired with what doctors and policy researchers say today. You’ll see how community health workers, local clinics, and small policy shifts can change outcomes. You’ll also find where cultural norms limit access, and why clear information matters. Sources include WHO, peer-reviewed studies, Mercatus analysis of ASHA programs, Frontiers research, Times of India reporting, and policy reviews. This article avoids technical jargon and focuses on what every reader should know: the facts, why they matter, and what concrete steps can widen access and improve outcomes. Read on for the eleven points that deserve more attention.
1. Maternal mortality has fallen overall, but big regional and social gaps remain

India has recorded steady declines in maternal mortality over recent decades, a public-health win that still hides large differences across states and communities. National improvements reflect better access to skilled birth attendants, emergency obstetric care, and wider institutional deliveries. Yet some districts and marginalized groups see much higher risks. Rural areas often have fewer facilities and longer travel times to comprehensive care. Economic barriers, caste and tribal marginalization, and weak transport or referral systems can turn routine complications into life-threatening situations. Tracking progress at the state and district level is crucial because national averages mask local problems. Local data and community engagement help health planners direct resources where they are most needed. For families, timely antenatal care and birth planning can dramatically reduce risks. While many women now deliver in clinics, maintaining quality of care and emergency readiness remains essential. Investing in trained staff, reliable supplies, and functioning referral pathways makes the decline in mortality real for every community, not just the better-served districts.
2. ASHA community workers drive measurable gains in service use

Accredited Social Health Activists, or ASHAs, are frontline workers based in villages and urban wards who connect families to health services. Research shows clear, measurable benefits: adding one ASHA per 1,000 population is associated with roughly a 2.04–4.1% increase in reproductive health service use. That’s not just a statistic — it means more women getting antenatal checkups, facility deliveries, contraception counseling, and follow-up care. ASHAs build relationships over time, earn community trust, and help translate medical advice into everyday actions, such as recognizing danger signs in pregnancy. Their long-term presence also helps change household behaviors that short campaigns struggle to shift. Challenges remain: training, fair pay, and supervision vary across states, and overburdened workers can burn out. Still, the ASHA model shows how community-based human connections can bridge formal health systems and households. Strengthening ASHA support, improving referral links, and recognizing their role formally in health planning can multiply these gains across districts that lag behind.
3. Many women still face gaps in contraceptive access and unmet need
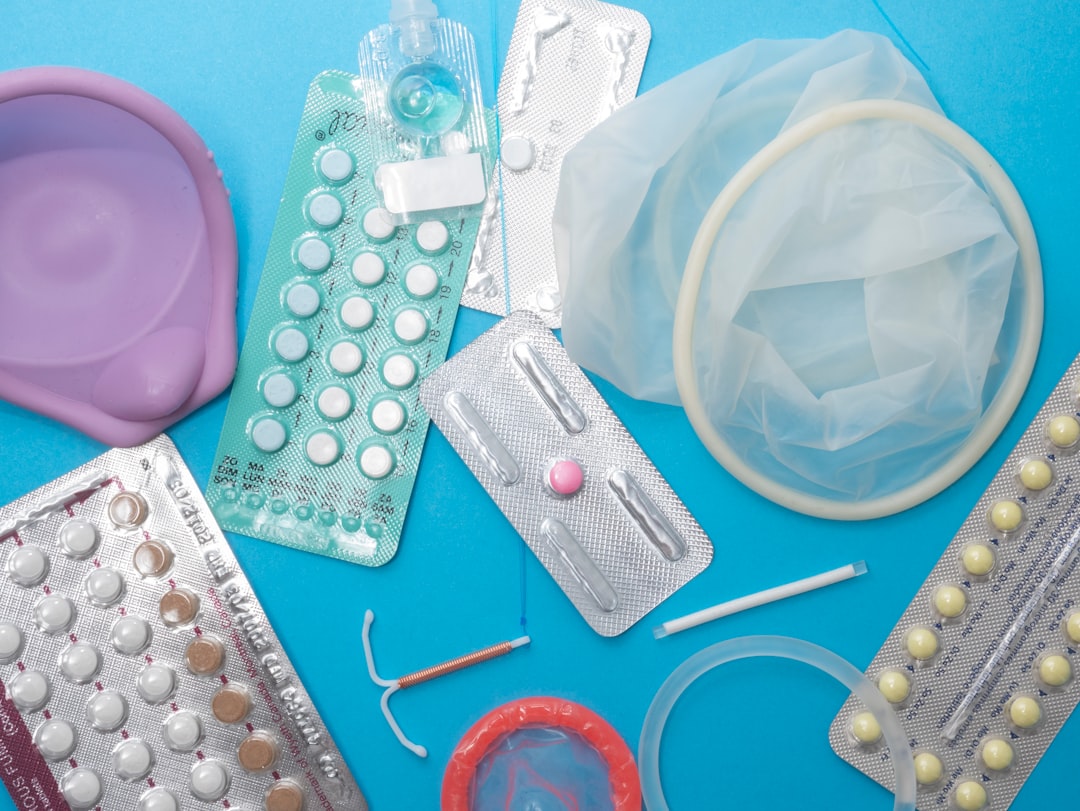
Despite improvements in service availability, many women in India continue to experience gaps in contraceptive access and informed choice. Unintended pregnancies remain a reality for millions, driven by inconsistent method supply, limited options in some facilities, and counseling that focuses narrowly on sterilization instead of a wider method mix. For reproductive autonomy to be real, women and couples need reliable information about options, side effects, and the ability to switch methods without judgment. Community outreach sometimes emphasizes a single approach, which can leave unmarried women, adolescents, and those seeking spacing methods underserved. Supply-side fixes—steady stock, trained counselors, and respectful clinic environments—matter. So do rights-based approaches that center consent and informed choice. Strengthening method availability at primary health centers and equipping ASHAs to provide accurate referrals can reduce unmet need. Clear counseling that explains how different methods work and how to manage side effects helps women stick with methods that suit their lives and goals.
4. Cervical cancer prevention and screening are underused despite clear solutions
Cervical cancer is largely preventable, yet screening and vaccination coverage remain low in many parts of India. WHO guidance emphasizes both HPV vaccination and regular screening as high-impact interventions, but access gaps and low awareness limit uptake. Screening can find precancerous changes early, and HPV vaccine programs can prevent most cervical cancers when delivered before exposure. Barriers include limited screening infrastructure in rural clinics, lack of trained staff, and social stigma or misinformation about tests and vaccines. Some programs have started mobile screening camps and community education drives, but scale and continuity are needed. Integrating cervical screening with routine reproductive health visits, training primary-care staff in simple screening methods, and making HPV vaccine available and affordable can change the picture. Engaging trusted community figures to explain the importance of screening and vaccination reduces fear, and tailoring messages to local language and concerns improves acceptance. With the right investments, cervical cancer should be an avoidable disease rather than a common cause of female mortality.
5. Fertility trends reflect complex lifestyle, environmental, and access factors

India has seen notable shifts in fertility patterns that reflect a mix of social change, lifestyle factors, and environmental influences. Urbanization, education, and changing family preferences have driven declines in average birth rates in many states. At the same time, reports note that lifestyle stressors, environmental exposures, and delayed childbearing influence fertility for some couples. Distinguishing demographic trends driven by choice from declines tied to health barriers is important. For example, when couples delay childbearing for education or work, fertility may fall by choice, whereas environmental toxins or untreated infections can reduce fertility involuntarily. Accurate local data and reproductive-health services that include fertility counseling can help couples understand options and risks. Public discussions often miss how work stress, nutrition, and exposure to pollutants can affect reproductive health, and this gap matters for planning health services. Awareness campaigns that explain modifiable factors, encourage early evaluation when couples face difficulties, and expand accessible fertility evaluation services increase the chances of timely, effective care.
6. Infertility is common but often stigmatized and misunderstood

Infertility affects many couples across India, yet cultural stigma and misinformation can make it a lonely and expensive journey. WHO highlights infertility as a public-health issue with emotional, social, and economic consequences. Many couples delay seeking care because of shame or the assumption that problems will resolve naturally. When they do seek help, cost and uneven availability of diagnostic and treatment services limit options, pushing some toward unregulated or costly interventions. Men’s role in fertility is often neglected, even though male factors contribute significantly to infertility. Expanding affordable diagnostic services at district hospitals, normalizing conversations about fertility in primary-care settings, and ensuring respectful counseling can reduce stigma. Community campaigns that explain that infertility has medical causes and that both partners may need evaluation help shift norms. Practical steps include training ASHAs and primary-care staff to recognize when to refer couples and building affordable public-sector fertility evaluation pathways so care does not depend solely on private clinics.
7. Adolescent reproductive health needs better information and safe services

Young people need accurate information and confidential services, but many adolescents lack access to age-appropriate sexual and reproductive health education in their schools and communities. Cultural sensitivities and local norms often limit classroom discussion, leaving young people to rely on peers or internet sources of mixed quality. Early marriage and early pregnancy remain realities in some regions, creating health risks for young mothers and their babies. Youth-friendly clinics, training for providers on confidentiality, and community dialogues that include parents and elders can open safe spaces for young people to ask questions and seek care. Practical programs combine school-based curricula with out-of-school outreach and helplines so adolescents who are not in formal education aren’t left behind. Ensuring access to contraception for those who need it, along with counseling that respects privacy, reduces the risks of unsafe abortions and early motherhood, and helps young people plan their futures with greater control and information.
8. Postpartum mental health is overlooked and under-resourced

New mothers often face emotional and mental-health challenges that go unrecognized in many communities. Postpartum depression and anxiety affect maternal well-being, infant care, and family dynamics, yet routine screening during antenatal and postnatal visits is not standard everywhere. Cultural expectations that a mother should be instantly joyful can add stigma, discouraging women from admitting distress. Community health workers, including ASHAs, can play a key role by spotting warning signs and offering referrals or basic psychosocial support. Low-cost group programs, peer-support circles, and training for primary-care providers on screening and brief interventions can make a difference. Mental-health services must be integrated into maternal care rather than treated as an optional add-on. Practical steps include adding short screening questions to routine visits, providing safe referral pathways, and ensuring community education that frames mental health as a common, treatable aspect of postpartum recovery.
9. Lesson for the US: community health workers can narrow access gaps

India’s ASHA program is a reminder that locally rooted health workers can move the needle on service use and health behaviors. In the United States, community health worker (CHW) programs have shown promise in reaching underserved populations, improving chronic-disease outcomes, and bridging cultural or language barriers. The ASHA experience underscores a few practical points for US programs: invest in sustainable pay and training, build clear referral links to higher-level care, and measure long-term behavior change rather than only short-term outputs. CHWs are most effective when communities trust them and when they are supported by functioning clinics and supply chains. For policymakers, funding CHW programs as part of routine primary care rather than temporary grants helps embed them in health systems. Evaluations should include both service-use metrics and measures of patient experience so the human value of CHW relationships is visible alongside clinical outcomes.
10. Lesson for the US: prioritize preventive screening and vaccination for durable gains
Cervical cancer prevention in India shows how screening and vaccines complement each other, and the lesson is global: prevention pays off. Countries that scale screening and HPV vaccination together see durable declines in cervical cancer. For the US and other high-income settings, maintaining high vaccination coverage and ensuring screening access for marginalized groups prevents avoidable disease. Outreach must reach those who face barriers, whether due to geography, language, or mistrust. Community-based vaccination drives, school-based programs, and making screening routine within maternal and primary care visits reduce missed opportunities. Investing in clear communication about benefits and safety, plus using flexible delivery models like mobile clinics, increases uptake. Preventive programs require sustained funding and coordination between public health, primary care, and community partners to convert scientific tools into population-level health gains.
11. Lesson for the US: tackling social norms and engaging men improves outcomes

Many reproductive-health outcomes improve when programs work with families, not just individuals. In India, successful interventions have engaged men in antenatal care, contraceptive counseling, and newborn care, helping shift norms about caregiving and responsibility. The lesson for the US and other settings is practical: involve partners in education, encourage shared decision-making, and design messages that speak to whole families. Programs that treat men as allies rather than obstacles reduce stigma around contraception and mental health support, and they increase support for maternal healthcare visits. Community dialogues, couple-based counseling when appropriate, and male-focused outreach in workplaces or community centers make involvement easier. By addressing gender norms directly and creating concrete roles for men in reproductive health, interventions achieve broader behavior change and more supportive household environments for women and newborns.
Conclusion: Awareness leads to better care, everywhere

India’s reproductive health landscape offers lessons that matter to readers everywhere. We see clear wins — falling maternal deaths and powerful community-based programs — alongside stubborn gaps in screening, contraception access, adolescent services, and mental-health care. These are practical problems, not mysteries, and many have practical solutions: stronger community-health-worker support, reliable supply chains, respectful counseling, and routine screening and vaccination. The three comparative items show that programs and policy choices in one country often translate into ideas useful in another, whether it’s the value of community health workers or the payoff from prevention and male engagement. For readers in North America, these lessons remind us to invest in relationships and systems as much as in technology. For readers connected to India, the findings suggest where attention, funding, and local advocacy can make the biggest difference. Awareness is the first step: share credible information, support accessible services, and encourage respectful, rights-based care. Small policy changes and consistent community action can turn facts into better outcomes for women, families, and communities everywhere.