8 Maternal Health Checkups You Should Not Miss
Pregnancy brings a stream of appointments that can feel overwhelming, but a handful of checkups make the biggest difference for your health and the baby’s. Start by booking a first prenatal visit as soon as you suspect pregnancy or have a positive home test; many providers aim for that visit near eight to ten weeks. Early visits set baseline measurements — blood type, hemoglobin, and initial screens — and create a personalised schedule for future testing. Routine visits continue throughout pregnancy, with timing that depends on risk factors and findings. A large recent study has called out maternal mental health as a major influence on pregnancy outcomes, so screening for depression and anxiety is increasingly seen as essential (Nature Medicine, 2025). For low-risk pregnancies some labs note a minimum of four antenatal visits, though many clinicians recommend more frequent checks later on (Metropolis Lab). This article keeps the title’s promise of “8 essential checkups,” then separates three closely related follow-ups into their own headings so you can see details and timing clearly. That means you’ll see eleven numbered sections below: eight core appointments plus three important, commonly scheduled follow-ups. Use this list as a conversation guide for your clinic — every pregnancy is different, and your care plan should be built with your clinician. If you want official schedules or specifics, ask your provider or check authoritative sources like ACOG and the CDC for U.S.-based guidance.
1. First prenatal visit (pregnancy confirmation and baseline health)

The first prenatal appointment is where pregnancy care begins and it often happens around eight to ten weeks when possible. Expect a review of your personal and family medical history, a physical exam, and basic checks like blood pressure, weight, and urine. Your clinician will usually order baseline blood tests that check for anemia, blood group and Rh factor, and certain infections, plus discuss folic acid and other supplements. This visit is also a chance to talk about medications you take and lifestyle habits such as diet and travel. If you have prior pregnancy complications or chronic conditions, your provider will outline a closer follow-up schedule. Use this appointment to ask practical questions — when to call for bleeding, how often to track fetal movement later on, or whether early genetic screening is recommended in your case. If you waited to schedule your first visit, don’t worry: an early visit is still valuable and helps put a clear care plan in place. Bring a list of medications, any prior records, and a support person if possible; practical details like clinic parking, language help, or telehealth options make the visit less stressful.
2. Early blood tests and baseline screens
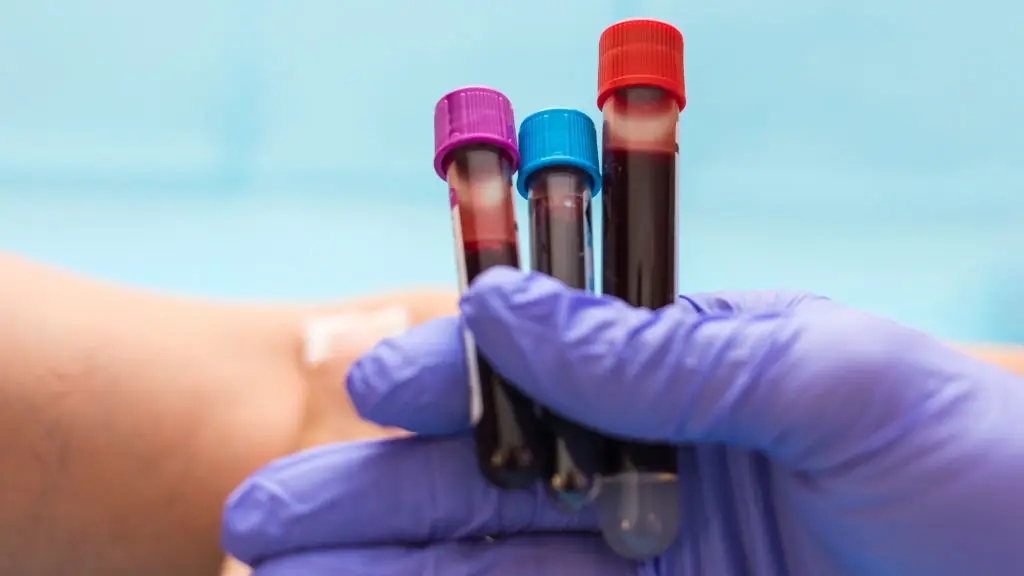
Early blood work gives a snapshot of your health and flags issues that can affect pregnancy care. Typical tests ordered at or soon after the first visit include a complete blood count to look for anemia, blood type and Rh status, and infectious disease screens that your provider deems appropriate. Knowing your Rh factor early matters because if you are Rh-negative and the fetus is Rh-positive, follow-up antibody testing and preventive measures may be needed. Baseline tests also let clinicians check thyroid function or immunity to illnesses like rubella when relevant. These labs guide whether you need supplements such as iron or adjustments to existing medications. Results can take a few days; clinics often use these findings to decide when to repeat tests or refer you to a specialist. Keep copies of your results and ask for plain-language explanations if anything is unclear. If you encounter access or cost concerns, ask the clinic about lab bundles, sliding-scale programs, or community health resources to make sure essential screens are completed.
3. Dating and early ultrasound

An early ultrasound does more than show a tiny heartbeat; it confirms the pregnancy location, estimates how far along you are, and rules out an ectopic pregnancy when needed. Dating scans are usually performed in the first trimester and help set the estimated due date — the date that guides timing for later screens and expected growth checks. The scan also confirms viability if you’ve had bleeding or pain. If multiple pregnancies are possible, the ultrasound clarifies whether you’re carrying twins or more. Technically, this appointment is quick but emotionally significant, so many people choose to bring a partner or family member for support. The sonographer captures images you can save, and the clinician will explain the basic findings and any follow-up steps. If the ultrasound is inconclusive, a repeat scan a week or two later often gives clearer information. Planning notes: wear comfortable clothing, and know whether your clinic asks for a full bladder for early scans — they’ll tell you when you book.
4. First-trimester chromosomal screening options
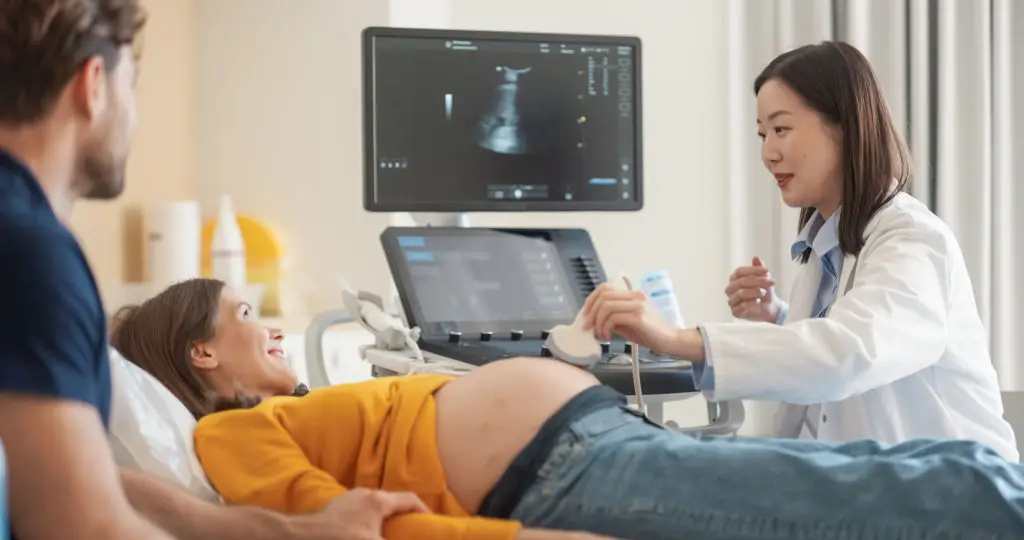
In the first trimester you may be offered screening options that estimate the chance of chromosomal differences. Typical approaches include combined screening, which pairs a blood test with a nuchal translucency ultrasound, and cell-free DNA testing (often called NIPT) that analyzes fetal DNA in maternal blood. These are screening tests, not definitive diagnoses; a positive screen usually leads to counseling and the option of diagnostic tests. Timing matters: combined screening is commonly done in the first trimester window, while NIPT can be offered a little later depending on your clinic. Screening helps families and clinicians anticipate needs and consider specialist referrals when appropriate. If results are concerning, your care team will discuss next steps, which might include genetic counseling. Remember that testing choices are personal — cultural values, family history, and personal priorities all play a role in deciding what to pursue. Talk openly with your clinician about what each test checks for, how reliable it is, and what support is available for follow-up decisions.
5. Mid-pregnancy anatomy scan (18–20 weeks)
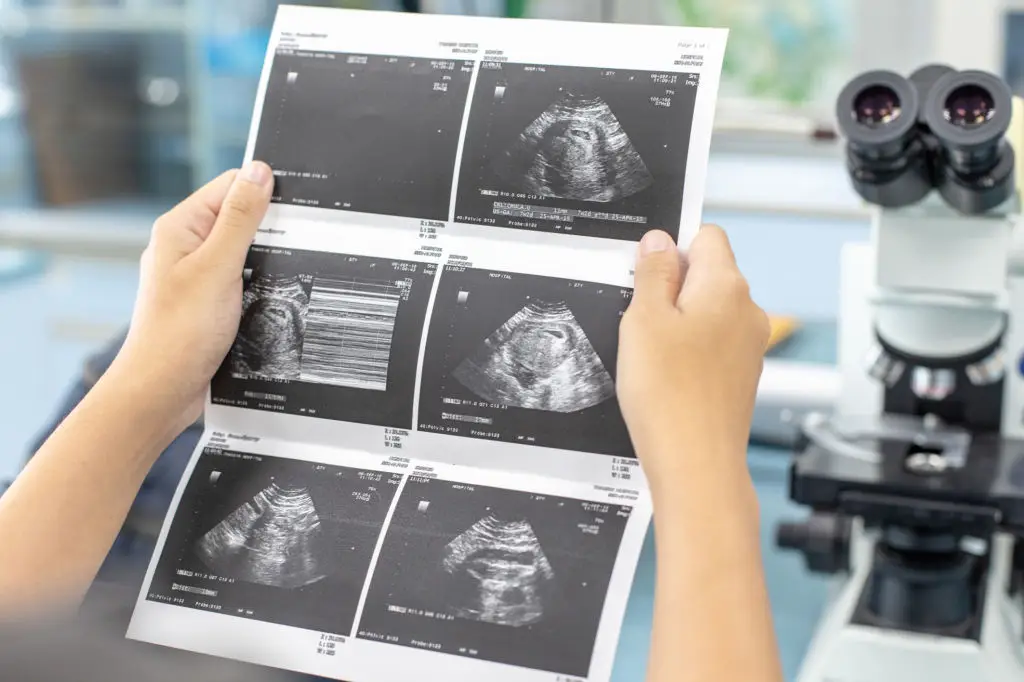
The mid-pregnancy anatomy scan is a detailed ultrasound usually scheduled around 18–20 weeks to review fetal anatomy and growth. During this scan the sonographer examines the brain, heart, spine, limbs, and organs, plus placenta placement and amniotic fluid volume. This window is important because many structural differences are best seen now, and findings influence later monitoring or referrals. The appointment can take longer than early scans because technicians measure and document multiple structures. Parents often find this scan emotionally rich: it’s a chance to learn the baby’s sex where permitted and to save images. If the scan shows a potential concern, your care team will explain what was seen, whether additional imaging or specialist input is needed, and the expected follow-up timeline. Even when everything looks normal, this scan provides reassurance and a clearer plan for growth checks in the third trimester. Practical tip: ask whether partners may attend in-person or by video, and consider bringing questions about your birth plan once the anatomy looks healthy.
6. Gestational diabetes screening (mid-pregnancy glucose testing)

Screening for gestational diabetes is a common mid-pregnancy check because untreated high blood sugar increases risks like larger birth size and delivery complications. Many clinics offer a glucose challenge test or a longer glucose tolerance test in the second trimester; the exact approach varies by practice. If screening shows high sugar levels, your care team will discuss dietary changes, glucose monitoring, and possible medication. Early lifestyle measures — adjusting meal composition and increasing gentle activity — often help and are recommended alongside medical follow-up. The goal is keeping blood sugar in a safe range to protect both parent and baby. If you have risk factors such as obesity, previous gestational diabetes, or a family history of diabetes, clinicians may screen earlier or more often. Ask your provider whether to do home glucose checks, how frequently to record results, and what thresholds will trigger treatment or specialist referral.
7. Maternal mental health screening

Mental health during pregnancy matters to physical outcomes and recovery after birth. Large research has shown strong links between antenatal mental disorders and obstetric complications, and experts have called for routine screening and management within prenatal care (Nature Medicine, 2025). Screening is typically done with brief questionnaires or direct conversation during visits, and clinicians can offer counseling, therapy referrals, or medications when needed. If you have a history of depression, anxiety, or trauma, flag this early so your care team can tailor monitoring and supports. Practical options include behavioral health referrals at the clinic, community mental health services, peer support groups, and low-cost counseling programs. Family members can help by encouraging check-ins and spotting warning signs like persistent sadness, trouble sleeping, or loss of interest in daily tasks. Remember that asking for help is a strength; treatment during pregnancy benefits both the parent and baby and often improves outcomes at delivery.
8. Blood pressure monitoring and preeclampsia checks

Regular blood pressure checks and urine protein screening are standard throughout pregnancy because they help detect preeclampsia early. Preeclampsia can develop after mid-pregnancy and requires prompt attention to lower risks for both mother and baby. Your clinician will track blood pressure at routine visits and may ask you to report any concerning symptoms such as sudden swelling, severe headaches, or vision changes. If elevated readings appear, your provider may increase monitoring, order blood work, or recommend medication and more frequent visits. Some clinics provide home blood pressure checks for higher-risk patients, which can help catch changes between appointments. Consistent monitoring is a practical way to prevent escalation and keep pregnancy on a safe course. If you have chronic hypertension, your care team will coordinate blood pressure goals and medication plans throughout pregnancy and after delivery.
9. Rh antibody follow-up and immunization review (supplement)
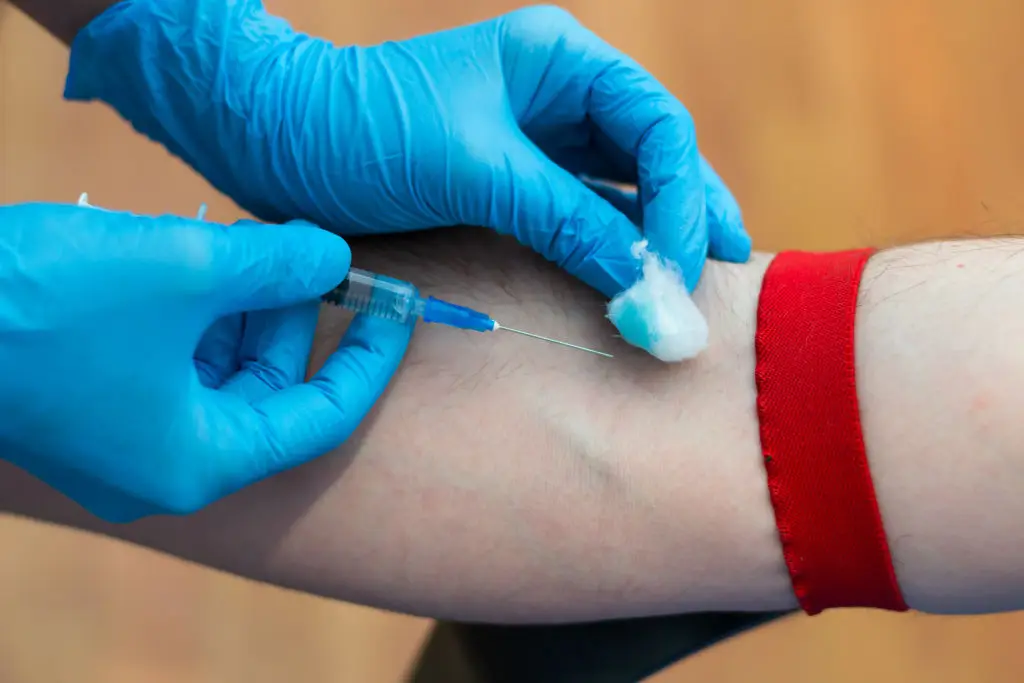
If your early blood tests show an Rh-negative blood type, follow-up antibody screening matters so your care team can prevent Rh sensitization in future pregnancies. Depending on results and timing, clinicians may discuss anti-D immunoglobulin as a preventive step. That follow-up is often scheduled in the third trimester and after events like bleeding or invasive procedures. This appointment also pairs well with a review of recommended vaccinations: seasonal flu shots are encouraged in pregnancy, and a Tdap dose in the third trimester helps protect newborns from pertussis. Talking through immunizations during a prenatal visit helps parents plan timing and understand benefits for the baby’s early weeks. If you have questions about vaccine safety or timing, ask your clinician for the latest guidance and resources.
10. Third-trimester fetal position checks and delivery planning
As the due date approaches, visits become more frequent to check the baby’s position, growth, and overall readiness for birth. From around the late second trimester into the third, clinicians watch fetal heartbeat patterns and may measure fundal height to assess growth. Near term, the focus shifts to whether the baby is head-down, breech, or transverse because position guides delivery conversations. This is also the time to firm up a birth plan — preferences for pain relief, who will be present, and contingency plans if induction or cesarean becomes necessary. Practical steps include touring the birth location, packing a hospital bag, and discussing signs of labor. If the baby is breech near term, clinicians discuss options like external cephalic version or planning a cesarean. Early, clear planning reduces stress and helps families feel ready for the big day.
11. Postpartum follow-up and early newborn planning

Postnatal care begins before birth by arranging an early postpartum visit and newborn checks. The postnatal appointment looks for wound healing when relevant, evaluates recovery from delivery, checks mental health, and supports breastfeeding and contraception planning. For many people, a postpartum check around six weeks is standard, but earlier visits or phone check-ins can be arranged if there are concerns. Planning ahead — lining up lactation support, pediatric follow-up, and community resources — smooths the transition. If you experienced complications during pregnancy, coordinate earlier postpartum monitoring with your clinician. Treat the postpartum visit as part of a continuum: good prenatal care sets the stage, but care does not stop after delivery. Bringing a partner, family member, or a checklist helps you cover physical needs and emotional concerns during that visit.
Wrap-up: Keep these checks on your calendar

Good prenatal care is a mix of timing, tests, and honest conversation. This article highlighted eight core checkups many clinicians consider essential, and three closely related follow-ups that commonly appear on prenatal schedules — hence the eleven numbered sections. Use the list to ask clear questions at each visit: what is being screened, why it matters, and what the next steps are if a result needs attention. If you want official guidance for scheduling or timing, consult U.S. professional resources such as ACOG and the CDC and bring those questions to your clinic. Remember that maternal mental health screening, routine blood pressure checks, and mid-pregnancy anatomy scans are not optional details — they are key pieces of a safer pregnancy journey (Nature Medicine, 2025). Practical touches help too: keep a small binder or digital folder with test results, bring a support person to important scans, and note any symptoms between visits so you can report them quickly. Every pregnancy is different, so use this as a flexible checklist rather than a rigid rulebook. When in doubt, call your care team early — timely checkups often mean simpler solutions and better outcomes for both parent and baby.