12 cancer screening tests India doctors recommend
Cancer screening saves lives when it catches disease early, but screening isn’t one-size-fits-all. In India a mix of public health drives, hospital programmes and private clinics offer different tests for different risks. National research shows screening rates are low in many regions, which makes clear, practical information useful for families deciding what to prioritise (NCBI/PMC studies). This guide lays out 12 cancer screening approaches that doctors in India commonly recommend — who they're for, how often they’re done, what to expect, approximate costs in public and private settings, and where to find local services (ICMR, Tata Memorial Centre).
1. Breast cancer screening: Clinical breast exam, mammography and ultrasound
Breast cancer is one of the most commonly discussed cancers in India. Doctors typically recommend regular clinical breast examination (CBE) from a younger age in community settings and mammography for eligible women. For average-risk women many oncology centres advise starting consideration of mammography around 40–50 years of age, with intervals commonly every 1–2 years; women with strong family history or known mutations may start earlier and follow a specialist's plan (Tata Memorial Centre; ICMR/NCCP guidance). In India, ultrasound is often used alongside mammography for younger women with denser breasts because ultrasound is radiation-free and useful for focal lumps. Public screening programmes or NGO camps may offer CBE free or at low cost. Private mammograms typically range (approximate) ₹1,500–5,000; public hospital costs are lower or subsidised.
2. Cervical cancer screening: VIA, Pap smear and HPV testing
Cervical cancer screening has clear options for different settings. Visual inspection with acetic acid (VIA) is a low-cost method used in community screening drives and can be followed by immediate treatment in some programmes. Cytology (Pap smear) remains widely available in clinics and hospitals, and high-risk HPV DNA testing is increasingly recommended where affordable because it detects the virus that causes most cervical cancers (WHO, ICMR). Many programs recommend starting screening in the mid-20s to 30s depending on sexual history and risk; a common international pattern is Pap every three years or HPV testing every five years for average-risk women aged 30–65. In India, cost ranges vary: Pap smear ₹300–1,500 in private labs, HPV tests typically ₹2,000–6,000; VIA is often offered free or low-cost at public camps.
3. Colorectal cancer screening: FIT and colonoscopy
Colorectal cancer screening is increasingly recommended where incidence is rising. The fecal immunochemical test (FIT) is a non-invasive stool test that checks for hidden blood and is often used as a first-line screen. A positive FIT usually leads to a diagnostic colonoscopy, which examines the colon directly and can remove polyps during the same procedure. Many doctors advise starting screening around age 45–50 for average-risk adults, earlier if there’s a family history. In India, FIT kits can cost about ₹300–1,000 from private labs, while colonoscopies in private hospitals typically range from ₹5,000–20,000 depending on sedation and facility; public hospital prices are lower or subsidised.
4. Oral cancer screening: visual oral examination

Oral cancer screening is especially important in India because of higher prevalence linked to tobacco, areca (betel) nut chewing and smokeless tobacco use. A simple visual oral examination by a trained clinician can find white or red patches, ulcers, or suspicious lumps early. Doctors recommend regular checks for anyone who uses tobacco or betel products, with opportunistic screening during dental or primary-care visits. Community screening camps and dental clinics may offer examinations free or at low cost. If a lesion is suspicious, a biopsy or specialist referral follows.
5. Liver cancer screening: ultrasound plus AFP for high-risk people
Doctors recommend targeted liver cancer surveillance for people at high risk: those with chronic hepatitis B or C, known cirrhosis, or certain metabolic liver diseases. The typical approach is abdominal ultrasound every six months, sometimes combined with the blood test alpha‑fetoprotein (AFP) to improve detection. This surveillance is not for the general population but for people with clear risk factors. In India, abdominal ultrasound at a private facility may cost ₹800–3,000; AFP blood tests add a few hundred to a couple thousand rupees depending on the lab; public hospitals may offer lower rates or programme-based screening for hepatitis patients.
6. Lung cancer screening: low-dose CT for high-risk smokers

Low-dose computed tomography (LDCT) screening reduces lung cancer mortality in well-defined high-risk smokers in clinical trials. In India, LDCT is offered primarily to high-risk individuals (longterm heavy smokers or those with strong exposure histories) and after shared decision-making because of false positives and radiation exposure. LDCT programmes are less widespread here than in some Western countries, and access varies by city and hospital. Costs for LDCT in private centres typically range from ₹5,000–20,000 depending on the facility; public hospital pricing may be lower.
7. Prostate cancer screening: PSA testing with careful discussion
Prostate-specific antigen (PSA) testing is widely available, but routine population screening is controversial because PSA can be elevated for reasons other than cancer and may lead to unnecessary biopsies. Many doctors in India follow a shared decision-making model: discuss risks and benefits with men aged 50 and above, or from 45 for those with family history or African ancestry. If chosen, PSA is a simple blood test; abnormal results may prompt referral to a urologist for digital rectal exam (DRE), repeat testing, imaging or biopsy. Private PSA tests typically cost a few hundred to a couple thousand rupees.
8. Skin cancer screening: visual checks and dermoscopy for suspicious lesions
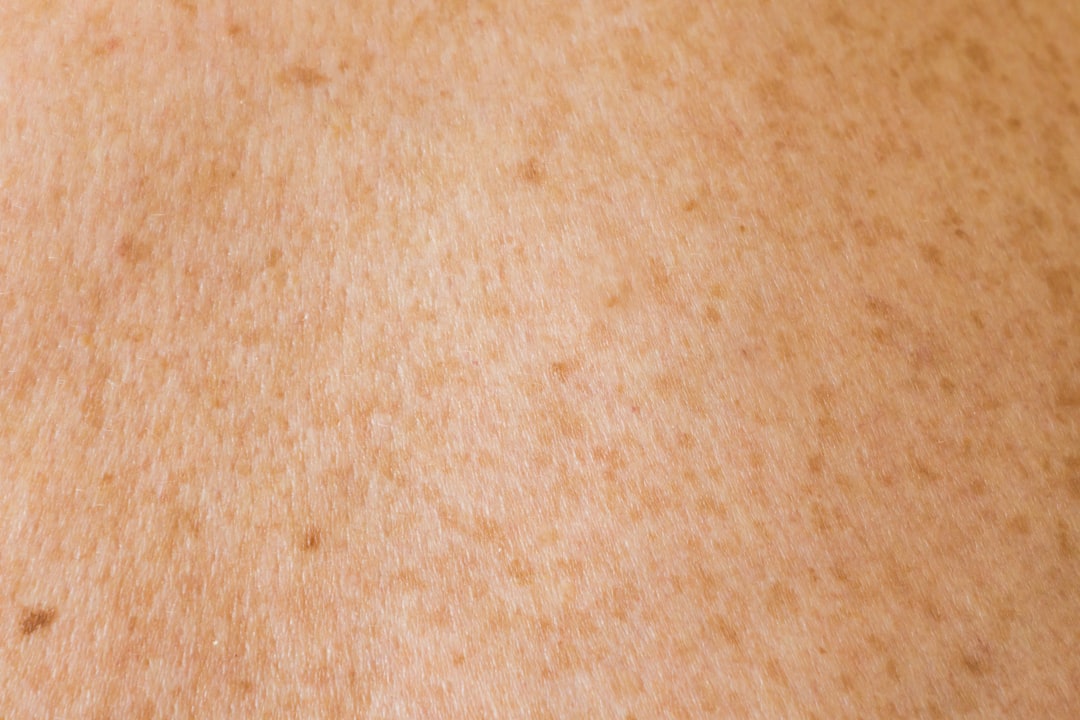
Skin cancer is less common in pigmented skin but still important to catch early. Doctors recommend people check their skin and see a dermatologist for any changing or suspicious moles, non-healing ulcers, or new rapidly growing lesions. Dermatologists may use dermoscopy (a handheld scope) for closer inspection and decide whether to biopsy. Routine population screening isn’t standard, but targeted checks are recommended for those with many moles, a family history of skin cancer, or significant sun exposure.
9. Genetic counselling and risk-based screening for families at high risk

When there is a strong family history of cancer (multiple relatives, early-onset cancers, or known gene variants), doctors recommend referral to a genetic counsellor. Genetic counselling helps identify whether targeted genetic testing is appropriate and which screening plan should follow — for example, earlier or more frequent breast and ovarian surveillance for BRCA mutation carriers. Genetic services are available at major cancer centres and private labs in India; testing and counselling costs vary widely, with tests costing several thousand to tens of thousands of rupees depending on the panel.
10. Opportunistic community screening: health camps and primary-care checks

Community screening camps and opportunistic checks at primary-care visits are an important way to reach people who may not seek hospital care. Typical services offered include CBE for breast screening, VIA for cervical screening, oral visual exams, and sometimes distribution of FIT kits. These programmes help detect early lesions and refer positives for diagnostic follow-up. Doctors advise anyone attending a camp to get clear instructions on follow-up pathways, because screening alone is not enough without timely diagnostics.
11. Tumor marker blood tests — why doctors usually advise against routine use
Blood tests that measure tumour markers (for example CEA, CA‑125, AFP, PSA) can be helpful in monitoring known cancer or guiding diagnosis, but many experts warn they are not reliable for routine population screening. False positives and false negatives are common; a raised marker does not always mean cancer and a normal marker does not rule it out. An ex-AIIMS oncologist and others caution against using marker panels as a screening shortcut (Indian Express reporting). Doctors usually recommend these tests only when there is a specific clinical reason, a suspicious symptom, or for follow-up after cancer treatment.
12. Smart health-check packages — what to choose and what to skip

Many private labs sell “full-body” health-check packages that bundle blood tests, imaging and specialist consults. Doctors advise picking packages based on age, risk and symptoms rather than buying the most expensive bundle. Sensible inclusions might be basic bloodwork (CBC, glucose, liver and kidney screens), targeted imaging when indicated, and age/risk-based cancer screens (for example mammography or FIT). Beware packages that promise tumour-marker panels as a general cancer screen; these are often not recommended without a clear clinical reason.
Wrapping up: how to use this checklist

Screening works best when it is personalised. This list gives 12 screening approaches doctors in India commonly recommend, with practical notes on who should be screened, how often, what to expect, and approximate costs. Start by weighing your age, family history, lifestyle (tobacco, alcohol, hepatitis risks) and symptoms, then discuss priorities with your primary doctor or a specialist at a recognised centre like Tata Memorial or an ICMR-linked clinic. Community screening camps are a good access point for several tests, but ensure you have a clear plan for follow-up if a test is positive.